The most recent PGEU Medicine Shortages Survey showed a continuing crisis that is causing patients to lose trust in their pharmacist and damaging staff satisfaction
Each year, the Pharmaceutical Group of the European Union (PGEU) conducts a survey among its membership to map the impact of medicine shortages across Europe from community pharmacists’ perspective.
The 2019 Survey was open to all PGEU member organisations and was conducted between 4 November-16 December 2019.
For the purpose of the survey, the term ‘medicine shortage’ was defined as every (temporally) inability for a community or hospital pharmacy to supply patients with the medicinal product requested as a result of factors beyond their control, requiring the dispensing of an alternative agent or even discontinuation of an ongoing medical therapy. In terms of reporting/notification of medicine shortages, respondents were asked to apply their national definition if available.
Among the key findings of the survey are:
• The high incidence and ongoing rise of the number of medicine shortages in most European countries;
• The daily and burdensome impact of medicine shortages on patients and pharmacy practice across Europe; and
• The existing gap in needed information, tools and legal solutions available to community pharmacists in many European countries for providing solutions to patients in case of a shortage.
The respondents were also asked, on average, per week, how much time pharmacy staff spend dealing with medicine shortages. While answers ranged from two hours to 15 hours per week, the average amount of time spent by pharmacy staff dealing with medicines shortages is 6.6 hours per week.
Other main findings from the survey include:
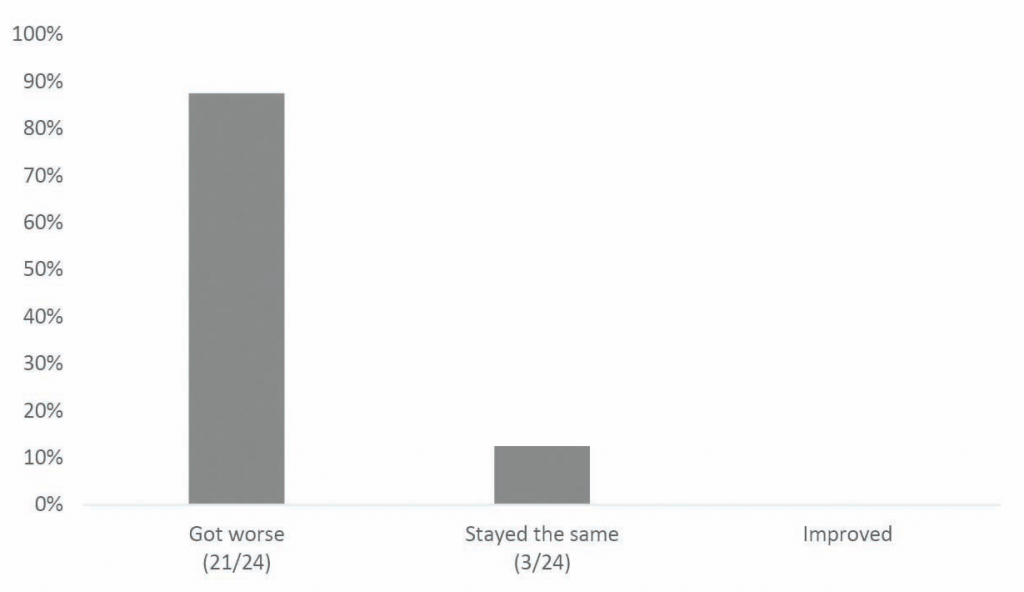
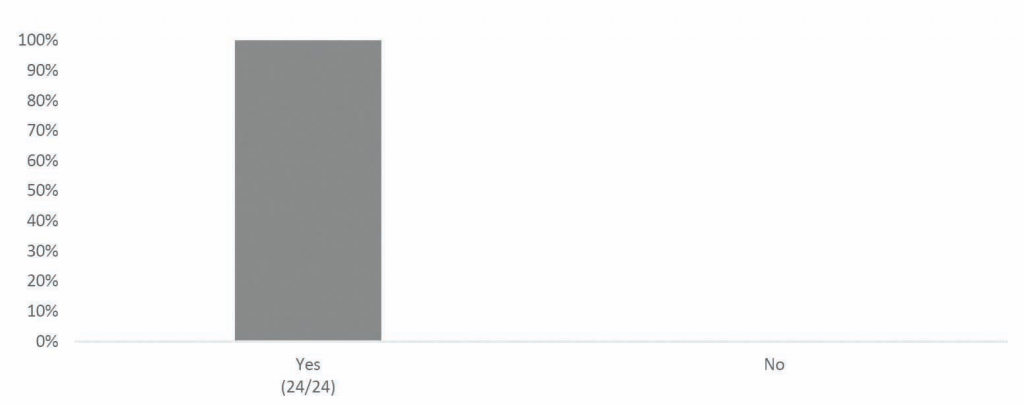
• All responding countries experienced medicine shortages in community pharmacies in the past 12 months, and in the vast majority (87 per cent) of countries, respondents indicated that the situation had gotten worse compared to 2018.
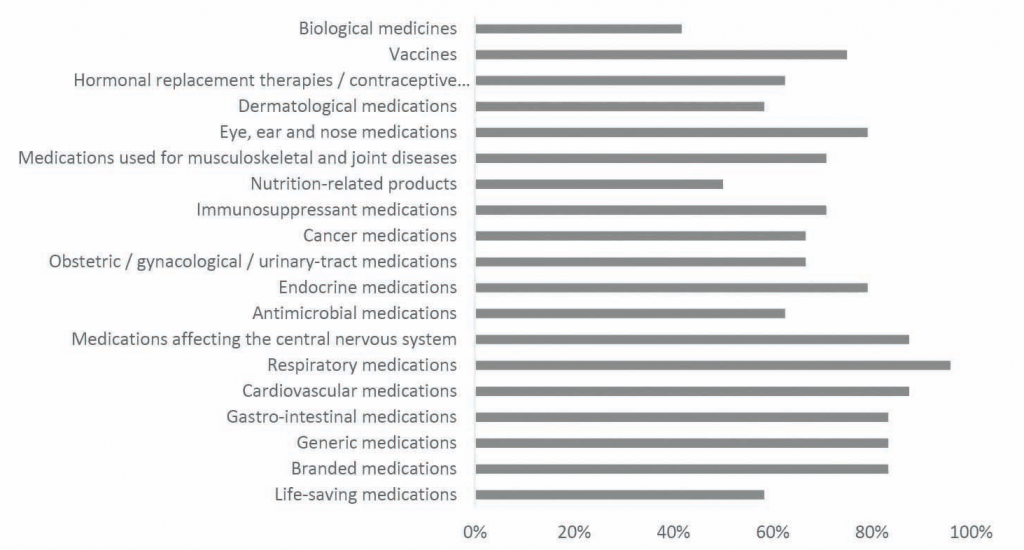
• All classes of medicines are affected by medicine shortages in community pharmacies across the different responding European countries. Respiratory medications have been short in supply in the highest percentage of countries (87 per cent), while biological medicines have been short in supply in the lowest percentage of countries (42 per cent).
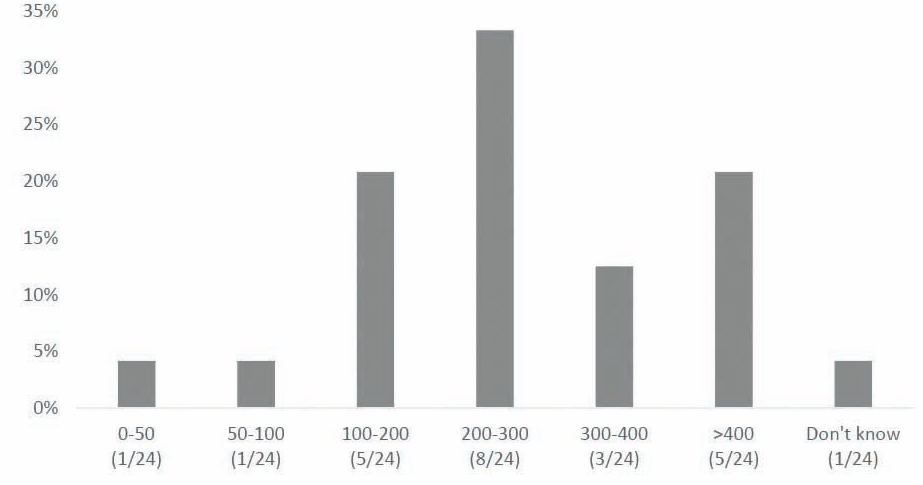
• In the majority of responding countries (67 per cent), over 200 medicines were listed as in short supply at the time of completing the survey, with five countries indicating that there were more than 400 medicines short in supply.
• All responding countries indicated that they believe medicine shortages cause distress and inconvenience to patients. Interruption of treatments (75 per cent of countries), increased co-payments as a result of more expensive/non-reimbursed alternatives (58 per cent), and suboptimal treatment/inferior efficacy (42 per cent) are also perceived as negative consequences of medicine shortages on patients.
• Medicine shortages are believed to affect community pharmacy businesses in most countries by reduced patient trust (92 per cent of countries), financial loss due to time invested in mitigating shortages (82 per cent), and reduced employee satisfaction (79 per cent).
• Across European countries, strong differences exist in terms of legal solutions community pharmacists can offer in case of a shortage. Generic substitution (79 per cent of countries), sourcing the same medicine from alternative authorised sources (such as other pharmacies) (63 per cent), and importing the medicine from a country where it is available (46 per cent) are the solutions which can be provided in most of the European countries. However, some of these solutions are subject to restrictions (ie, new prescription is needed) and can be cumbersome and time-consuming for the patient and the pharmacist.
• 25 per cent of responding countries indicated that there is still no reporting system for shortages in place which can be used by community pharmacists in their country, despite that pharmacists often experience or foresee supply difficulties before the industry or wholesalers are aware that there is, or will be, a problem.
• Community pharmacists receive their needed information on shortages in most countries from wholesalers (71 per cent), medicines agencies (67 per cent) and pharmacy organisations (42 per cent).
Mr Darragh O’Loughlin, General Secretary of the Irish Pharmacy Union, commented on the survey results: “The release of this survey underlines that medicine shortages are an increasing challenge, not just in Ireland, but across Europe.
“In Ireland, we have experienced significant shortages of medicines in the last year and the situation continues to get worse. Patients can sometimes wait for weeks to get a new supply of a common drug. Not only is this putting their health at risk, but it is causing undue stress, fear and anxiety for patients. Instead of directing their efforts and professional expertise towards the needs of patients, pharmacists are spending nearly seven hours a week resolving medicines shortages and firefighting on behalf of our patients.”