Anna Wedderburn presents an overview of the need for adequate folate intake and its effects on overall health
Folate, also known as vitamin B9, is a water-soluble vitamin that is obtained through diet. Folate was first isolated in 1941, and it is now known to play an important role in the synthesis of DNA and RNA, the methylation of DNA, the metabolism of amino acids, and the formation of red and white blood cells.
This vitamin allows for healthy and fully-functional cell division, and is therefore of particular importance during periods of rapid growth and development, such as pregnancy. It is also thought that folate plays a role in mental health and cardiovascular health, among other aspects of health. There is a man-made version of folate, known as folic acid. Folic acid is much more stable than folate, and is more bioavailable within the body. For this reason, naturally-occurring folates in foods are limited in their ability to influence blood folate levels.
Folate is absorbed into the bloodstream from the gut. From here, it moves to the liver for processing. Any excess folate passes to the kidneys and is then excreted from the body as urine. Folate is naturally present in a wide variety of foods, including: Liver, dark leafy vegetables, legumes, egg yolk, avocado, asparagus, and broccoli.
Health risks associated with low folate levels
Mental health
A low folate status has been linked to an increased risk for depression and a poor response to antidepressant treatment. Although folic acid does not appear to be as effective as an antidepressant by itself, supplementation does appear to boost the impact of antidepressants in some individuals, particularly in women who are taking fluoxetine. Low folate has also been associated with schizophrenia, dementia, Alzheimer’s disease, and anxiety.
Cardiovascular disease and stroke
High levels of homocysteine in the body is associated with an increased risk for cardiovascular disease and stroke. Folic acid supplements have been demonstrated to lower levels of homocysteine in the blood, potentially reducing the risk of cardiovascular disease and stroke. However, there is still controversy surrounding the role of folate in preventing cardiovascular disease and stroke, with some studies yielding conflicting results.
Megaloblastic anaemia
A lack of folate within the body can lead to megaloblastic anaemia. In megaloblastic anaemia, red blood cells do not form properly — they are larger than normal, are oval-shaped instead of round, and there are fewer of them. Symptoms include pale skin, decreased appetite, irritability, fatigue, diarrhoea, and a smooth and tender tongue.
Pregnancy and neural tube defects
The importance of folate in the development of an embryo during pregnancy was discovered in 1991. Folate deficiencies prior to and during the early stages of pregnancy can lead to neural tube defects in offspring. In an embryo, the neural tube is the structure that develops into the entire nervous system. Neural tube defects occur in embryos 21-to-28 days after conception, at a time when most women do not know they are pregnant.
Women who are deficient in folate are more likely to give birth to children with neural tube defects such as anencephaly (absence of a major portion of the brain and skull), encephalocoele (sac-like protrusions of the brain and the membranes that cover the brain through openings in the skull), and spina bifida (underdeveloped spinal cord and backbone). The optimal folate status for neural tube defect protection is greater than 907nmol/L.
As neural tube formation occurs so early in embryonic development, it is recommended that women take 400ug of folic acid a day three months prior to conception, and for 12 weeks into pregnancy. It is important to note that these recommendations specifically refer to folic acid supplements, as folic acid is more bioavailable than folate, as opposed to relying on naturally-occurring folate within foods.
It has been demonstrated that folic acid supplementation can reduce neural tube defects by up to 70 per cent. As folic acid has such a significant role in preventing neural tube defects, it is actually recommended that all women of reproductive age and who are sexually active take 400ug of folic acid daily, as from the years 2014 to 2019, there were 121 million unintentional pregnancies annually across the globe.
Ireland is not exempt from this. Studies have reported that only 40-to-45 per cent of pregnancies in Ireland are planned, while uptake of folic acid in Ireland has been reported to be low during pregnancy, and even lower prior to conception. In a study in 2015, it was found that in Ireland, only 36 per cent of women of reproductive age had levels of folate in their blood that would be considered to be protective against neural tube defects. Furthermore, almost 50 per cent of the indigenous Irish population have variations in a gene that codes for an enzyme involved in folate metabolism.
These variations decrease the body’s ability to metabolise folate, contributing to an increased risk of folate deficiency. This genetic mutation, alongside the low levels of folic acid supplementation in women in Ireland, perhaps makes it unsurprising that the rates of neural tube defects in Ireland are among the highest in the world.
Fortification of foods, such as flour and cereals, with folic acid is mandatory in some countries. This has a significant impact on incidence of neural tube defects. In Canada, the US and Chile, for example, mandatory fortification of these food types led to a 27-to-50 per cent decrease in rates of neural tube defects.
In Ireland and most other EU countries, fortification of foods with folic acid is not mandatory, but fortification of foods with folic acid is thought to reduce the risk of neural tube defects by 11-to-14 per cent. The statistics surrounding folate levels and pregnancy in Ireland suggest that there is a lack of awareness in women who are of reproductive age when it comes to the importance of folic acid for embryo development, particularly prior to conception. This is where pharmacists have the potential to play an important role in raising awareness.
It is unlikely that women who are thinking about becoming pregnant will schedule an appointment with their doctor to discuss pregnancy, unless they are having issues with conception. It is quite likely, however, that they or their partner will visit a pharmacy to buy a pregnancy test. This could provide a good opportunity to discuss the importance of folic acid in the lead-up to pregnancy, particularly if the individual buying the pregnancy test has questions about what supplements they or their partner should be considering.
Recommended amounts of folate intake
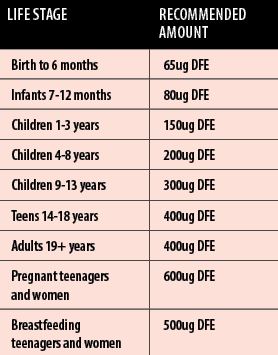
The recommended daily allowance for folate for the different demographics is listed in the table on the previous page. The allowances are based on the ‘dietary folate equivalent’ (DFE) unit. DFEs are used as folic acid has a higher bioavailability than folate that is found in food. It is estimated that 85 per cent of folic acid taken with food is bioavailable, whereas approximately 50 per cent of folate naturally present in food is bioavailable. Based on these bioavailabilities, DFEs are defined as follows:
- 1ug DFE = 1ug food folate.
- 1ug DFE = 0.6ug folic acid consumed with food.
- 1ug DFE = 0.5ug folic acid on empty stomach.
Women who have a history of neural tube defects in their family are advised to take more than the recommended amount of folic acid stated above. Women with this medical history should discuss folic acid supplementation with their doctor prior to conceiving. The doctor may decide to give them a prescription for a supplement with a higher concentration of folic acid. It is recommended that folic acid supplements should not be given to infants under the age of one, unless advised by a healthcare professional to do so.
Folic acid supplements
Over-the-counter vs prescription
Folic acid is available as a prescription, but also as an over-the-counter medication. In most cases, over-the-counter folic acid supplementation is sufficient. Prescription folic acid supplements contain a higher concentration than over-the-counter supplements, and are used for individuals severely deficient in folate, those with absorption issues, or in women who have a family history of neural tube defects. The over-the-counter folic acid supplements, such as Clonfolic tablets, generally contain 400ug of folic acid.
Side-effects
There are potential side-effects to taking folic acid, although they are rare. They include nausea, loss of appetite, bloating, and wind. Toxicity from folic acid is even more rare, although high-dose supplementation is still not advised unless under medical supervision. As folate is water-soluble and readily excreted from the body in the urine, overdoses are not a major concern.
Allergies
Allergic reactions to folic acid are extremely rare. The reactions that have been reported include erythema, skin rash, itching, general malaise, and respiratory difficulty.
Interactions with other medications
Although folic acid supplementation is advisable and considered to be very safe, it may interact with the following medications:
- Anticonvulsants: Folic acid might decrease the blood concentration of drugs such as fosphenytoin (Cerebyx), phenytoin (Dilantin, Phenytek) or primidone (Mysoline).
- Barbiturates: Folic acid may decrease the effectiveness of central nervous system depressants.
- Methotrexate (Trexall): Folic acid could interfere with the effectiveness of this medication used to treat cancer.
- Pyrimethamine (Daraprim): Folic acid may reduce the effectiveness of this drug.
References on request







