The Citizens’ Jury on Access to Health Information reveals patients’ feelings on how their information is handled and accessed by healthcare professionals and shows a lack of trust in the State.
The results of the consultation, which was organised by the Irish Platform for Patient Organisations, Science and Industry (IPPOSI), were released last month and set out six recommendations for policy-makers. The participants also expressed a strong preference for greater access to health information in Ireland. They also underlined that health information must not only be easily accessible to every citizen who wants to view their information, but that citizens must also be able to actively manage and consent to the use of their information on an ongoing basis.
In addition, the CEO of IPPOSI highlighted to this publication the need for pharmacists to have access to patient’s health records in order to ensure continuity of care. The panel of ‘jurors’ consisted of 25 people who deliberated for 12 hours on the following two questions:
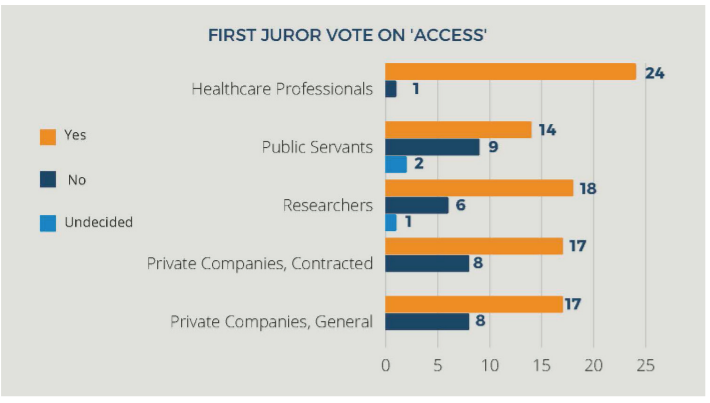
1) Who should be able to access, share and use your health information (identifiable and non-identifiable) and for what purpose(s)?
The options for a response were:
a) Healthcare professionals in public or private settings (hospitals, GP, community health, social care) seeking to access health information to support service improvement, change, innovation;
b) Public servants in Government departments and agencies (ie, HIQA, HPRA) seeking to access health information to support legislative, policy or practice change;
c) Researchers (academic or clinical) seeking to access health information to complete health research, with the appropriate ethics approval (publicly or commercially sponsored) to conduct health research or develop health innovation;
d) Professionals from private health companies, contracted by the public sector, seeking to access health information;
and e) Professionals from private health companies seeking to access health information to conduct health research or develop health innovation (medicine, device, vaccine).
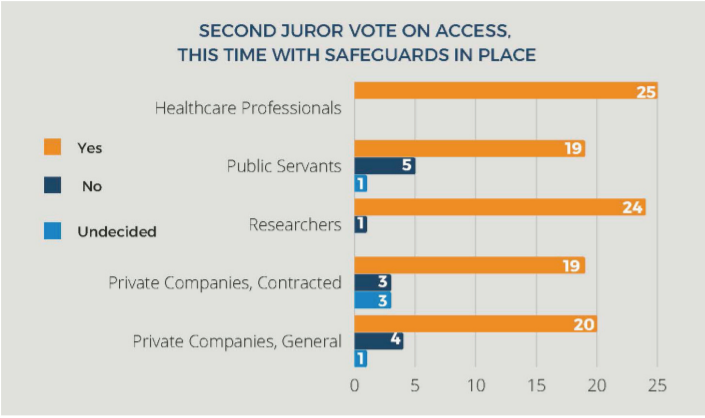
2) Are there provisions which would increase your trust and confidence in different stakeholders accessing, sharing and using your health information?
The respondents could choose from:
a) Being able to view what health information is available about you (ie, see your own health data);
b) Being able to view who has accessed your health information;
c) Being informed about how your health information is kept secure;
d) Having more information about the benefits of sharing health information;
e) Having more information about the potential future uses of sharing health information;
f) Being able to withdraw from/opt out of sharing your health information;
g) Being able to consent to/opt in to sharing your health information;
h) Being able to control who accesses your health information;
i) Being able to request the destruction of your health information after use;
j) Having more public and patient involvement where decisions are being made around who can use health information and why;
and k) Being confident that sanctions exist and will be applied where health information is misused.
The jurors concluded that they have a lack of trust in the State because of past failings in relation to health information collection and use. They also spent time discussing the potential for data breaches, and called for robust cyber security solutions and safeguards to protect their health information and a zero-tolerance approach to the misuse of health data. Overall, they stressed the importance of:
Health records: Health information should contain up-to-date, complete, joined-up data which provides an accurate and comprehensive account of the individual’s history of contacts with the health service and his/her health record.
Portal: Information sharing should be via a portal that is equally accessible to both the patient and the healthcare professionals engaged in their care.
‘Closed box’: Information sharing should be limited, both in terms of what information can be viewed (closed box) and in terms of who can view the information (audit trail).
Citizen first: Health information must be first shared with every citizen who wants to view, and potentially control access to, their own health information.
Public champion: Health information sharing needs to be guided by an independent, State-mandated, public champion who acts in the interest of the citizen, and who is responsible for informing, educating, empowering, and protecting the public.
Inappropriate sharing: Health information should never be shared with employers, banks, or insurance, pension, and marketing companies.
Price to pay: Health information should not be given away ‘for free’, instead it should be treated as a modern-day ‘national resource’ from which society must accrue a tangible, financial benefit (or in-kind benefit) for sharing.
Sanctions: Health information misuse should be approached from a position of zero-tolerance, especially misuse from within the system, in particular by public servants outside of healthcare professionals.
Security: Health information must be appropriately secured by the State, and sufficient resources dedicated towards its security.
Commenting on the results, Dr Derick Mitchell, CEO of IPPOSI, stated: “A Citizens’ Jury on access to health information is very topical for a number of reasons — the initial rollout of the Covid-19 vaccine programme and the need to access records to identify priority groups; the subsequent development of a vaccine portal and the creation of the EU Digital Covid certificate; and, of course, the recent cyber attack on our national health system. People are worried about their data. They want to know who has it and who is in charge of protecting it but, more importantly, they want to play a central role in deciding what happens to it.
“Jurors expressed a clear desire for a connected, quality, digital health information system, and the need for accountability and independent oversight of our health information. Jurors also concluded that the sharing of health data for the improvement of patient care is a collective responsibility and ultimately the right thing to do, subject to the conditions set out.
“Our jurors have started the discussion, and we in IPPOSI believe it is up to the health policy-makers and decision-makers to take this further and start a national conversation about the future of our health information to deliver on this collective call for action.”
Dr Mitchell also commented to Irish Pharmacist (IP) on the need for pharmacists to have access to patients’ health records. “The jury members expressed a strong desire for a joined-up health record, recognising the need for healthcare professionals to have access to this complete picture of an individual’s health information, in order to provide quality, evidence-based, real-time care to individual patients,” he said.
“The jury went even further by highlighting that access (for both professionals and citizens) could be managed via an online portal, whereby appropriate access can be managed securely and according to the patient/citizen consent, even for purposes beyond individual care. As one of the most publicly trusted healthcare professions, I believe pharmacists are a group of healthcare professionals who could help contribute to developing these portals and associated consent models for both individual care and for so-called ‘secondary purposes’.
“It is also noteworthy that the jury appealed for citizens to be involved in the broader, strategic-level decision-making around health information management (ie, outside their involvement in the management of their own information) with specific calls for patient involvement in governance, oversight, and advisory mechanisms.” ?







