A clinical overview of Roscrea, including subtypes and treatment and the potential to confuse it with other conditions.
Rosacea is an inflammatory skin disease causing facial flushing, redness, papules, pustules and in
some cases permanent dilation of small blood vessels (known as telangiectasia). The cheeks, chin, forehead and nose are usually the worst affected, with the rest of the face mainly unaffected. Rosacea can be temporary in
some cases, but is often recurrent or persistent. There are four subtypes of rosacea. It is sometimes referred to as acne rosacea; however, this can cause confusion, as rosacea is unrelated to acne vulgaris. Rosacea is mostly diagnosed in people aged 40-to-59 years and is rare in people aged under 30.
Prevalence
Worldwide estimates of prevalence vary widely, from 1-to-22 per cent. It is often referred to us the ‘Curse of the Celts’, as it is especially prevalent in people of Celtic and especially Irish decent. For example, in a study done in the USA, 33 per cent of those with rosacea reported at least one parent of Irish ancestry, despite only 15 per cent of the US population being of Irish decent. Despite its association with Celtic people, rosacea also occurs in populations with darker skin tone. Its prevalence in the UK is 10 per cent and in Ireland, is 15 per cent of the population.
Causes
The exact causes of rosacea are not known. Causes are a complex mix of genetic and environmental influences. A genetic cause has not been found; despite this, studies suggest that people with rosacea are four times more likely to have a family history of the disorder than people without the condition. The immune system also has an influence in causing rosacea. High levels of cathelicidins are present in patients with rosacea. Cathelicidins are antimicrobial peptides that are part of the innate immune system that cause neutrophilic infiltration of the dermis and dilation of blood vessels, causing oedema and inflammation.
Ultraviolet (UV) radiation from sunlight has a pro-inflammatory effect, which explains why sunlight exacerbates symptoms of rosacea. UVA light causes collagen denaturation and activates an inflammatory response. UVB light promotes release of fibroblast and vascular growth factors, which increase blood vascularity. Higher levels of matrix metalloproteinases (MMPs), including collagenase and elastase, increase inflammation and are seen in patients with rosacea, which may be a factor in causing the thicker and harder skin.
Other factors, including heat or capsaicin in foods, can increase flushing and burning. Increased water loss in the epithelium results in decreased epidermal hydration for rosacea patients, which worsens symptoms, as it reduces the skin’s barrier function.
Influence of skin bacteria
Patients with rosacea have been shown to have higher counts of Staphylococcus epidermidis and the hair follicle
mite Demodex folliculorum, which promote inflammation. Bacillus oleronius has also been linked to rosacea, probably due to increased inflammatory cytokine production.
Helicobacter pylori, a common bacteria found in the gastrointestinal tract, has been shown to have a higher
prevalence in the gastrointestinal tract of rosacea patients. H.pylori increases levels of nitrous oxide in the blood and tissues, which is the reason it seems to increase erythema (red inflamed skin) in rosacea.
Diagnosis
Blood tests or skin biopsies are not needed to diagnose; diagnosis is based on physical signs and symptoms. Identifying triggers to be avoided should be part of the diagnosis process.
Symptoms
These include dry, flaky, sensitive skin that burns or stings when facial creams like sunscreen or make-up are applied. Rosacea increases risk of blepharitis, sore and inflamed eyes, swelling of facial areas and can risk development of an enlarged nose (rhinophyma) with prominent pores (sebaceous hyperplasia). The area around the eyes is unaffected, though the eyelids are often affected.
It is more common in women but tends to be more severe and peaks later in men. Rosacea tends to effect women more on the cheeks and chin, while men are more likely to have rhinophyma. Rosacea can result in self-consciousness and embarrassment that can lead to social anxiety and depression. Therefore, it is important that rosacea is not dismissed as either trivial or a simple cosmetic issue.
Blood tests or skin
biopsies are not needed
to diagnose; diagnosis
is based on physical
signs and symptoms
Primary symptoms: Erythema, pustules, and telangiectasia
Temporary facial flushing similar to blushing or sunburn in the centre of the face is often the first sign of rosacea. This is due to vasodilation. This erythema (flushing) generally becomes more permanent and noticeable with time, with swelling often developing.
Rosacea diagnosis requires one or more of the primary symptoms, which are:
Transient erythema, ie, flushing.
Non-transient erythema.
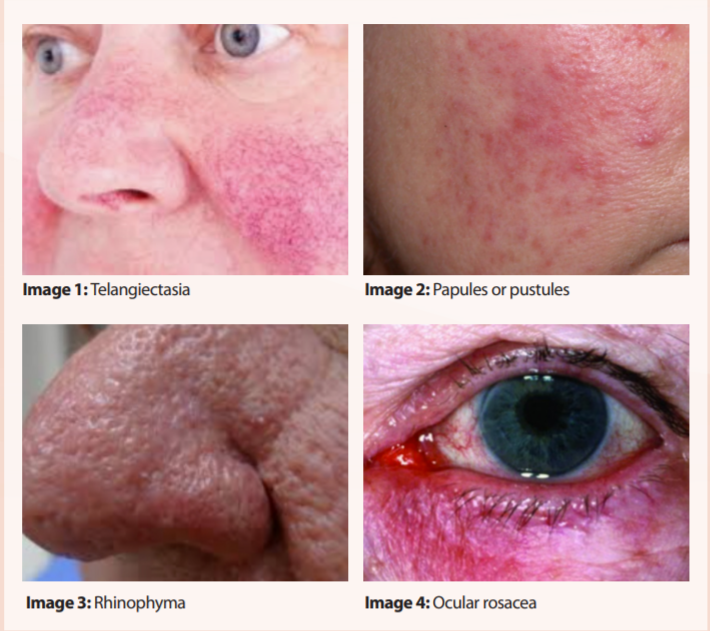
Telangiectasia: See image 1.
Papules or pustules: See image 2.
Secondary symptoms
Secondary features can include a burning or stinging sensation, dry skin, oedema, phymatous changes, ie, thickened skin, lump-like nodules and enlarged, red and bumpy nose, known as rhinophyma (see image 3).
Ocular Rosacea
Approximately half of people with rosacea have symptoms affecting the eyelids or eyeball (see image 4). Symptoms include watery or bloodshot eyes, dry eyes, burning, stinging or itchy eyes, blurred vision, sensitivity to light, and recurrent styes. Ocular rosacea is also associated with conjunctivitis, anterior blepharitis, including irritation of eyelash bases and eyelid margin, and posterior blepharitis, which affects ducts and eye secretions, and meibomian cysts (small swellings on either the upper or lower eyelid, or on both). Symptoms of more severe ocular rosacea include keratitis, iritis, episcleritis and scleritis.
Conditions with similar symptoms
Acne vulgaris: New-onset acne vulgaris is uncommon in older populations. If open and closed comedones (blackheads and whiteheads) occur, then acne ]=-vulgaris is more likely, as they do not occur with rosacea. People with acne tend to have more greasiness of the skin. Involvement of the chest and back is often a feature of acne, but this is not the case in rosacea.
Contact dermatitis: Irregular distribution and recurrent episodes of blistering with swelling, or red, dry plaques
may indicate contact dermatitis.
Seborrhoeic dermatitis: Presents as erythema and scaling, with some itch. Seborrhoeic dermatitis most commonly
affects the lateral sides of the nose and the nasolabial folds (skin folds that run from each side of nose to corner of mouth), eyebrows and glabella (area of the forehead above and between the eyebrows).
Rosacea fulminans: Rosacea fulminans occurs more in young women after puberty and resembles rosacea or severe acne, but flushing does not occur.
Steroid rosacea: Due to overuse of topical steroid creams. The symptoms are similar to conventional rosacea, making it difficult to distinguish.
Subtypes of Rosacea
The four subtypes are not an indication the condition is worsening, and patients can have more than one subtype at any one time. They are:
Erythematotelangiectatic rosacea (Image 1):
Frequent episodes of transient facial erythema (flushing) and non-transient, or persistent erythema. Associated with facial oedema, burning, or stinging and rough or scaly skin.
Papulopustular rosacea (Image 2):
Includes ‘whitehead’ pustules and red, swollen bumps which typically occur on the cheeks, chin, and forehead and can be mistaken for acne. Facial redness and flushing may appear too, but people with papulopustular rosacea tend to have less flushing.
Phymatous rosacea:
Thickening of the skin and uneven surface nodularities on the nose, forehead, chin, ears and eyelids.
Ocular rosacea (Image 4):
Described above.
Treatment
Non-pharmacological options There are triggers which may not be the primary cause, but may exacerbate
symptoms. They should be identified and avoided. Triggers can include sunlight, temperature extremes, wind, stress, spicy foods, hot drinks, alcohol and some drugs, such as topical corticosteroids, vasodilators such as nicotinic acid.
General advice:
Moisturise regularly, especially if skin is dry, ie, non-greasy emollients that reduce moisture loss and reduce roughness.
Wear sunscreen. Some patients benefit by use of a high-factor sunblock (factor 30+) all-year-round.
Placing ice between cheek and gum can reduce erythema short-term.
Reduce spicy foods, alcohol, and hot showers.
Ease blepharitis from ocular rosacea with: Warm compression and gentle massage of the eyelid margin; cleaning the eyelid with a cotton bud or along the eyelid margin with diluted baby shampoo; avoiding cosmetics around the eye, especially eye-liner.
Preservative-free ocular tear substitutes are best to treat dry eyes.
The pharmacological treatment of rosacea
Topical treatments are first choice for mild rosacea and oral treatments should be reserved for moderate-to severe rosacea. The UK’s Primary Care Dermatology Society (PCDS) published Rosacea: A primary care treatment pathway in 2016. It identified that patients with rosacea often end up on prescribed antibiotics for many years; however, now that very effective non-antibiotic alternatives are available, the PCDS were keen to endorse the use of non-antibiotic treatments to help reduce risk of antibiotic resistance. For example, in the UK, it is estimated that 8 per cent of all antibiotics prescribed are for dermatology indications.
Tropical Rosacea Treatments
Metronidazole cream: Topical metronidazole’s ability to treat rosacea is due to its anti-inflammatory properties instead of its antimicrobial effects. It can be used short-term for a flare-up or longer-term for more persistent cases, or combined with oral medication in persistent or severe rosacea. Topical metronidazole should be applied to affected areas twice daily for three-to-four months to experience maximum benefit. This benefit can last for three-tosix weeks after treatment but in some cases can give remission for up to six months after treatment. Side-effects of topical metronidazole can include dry and irritated skin, but side-effects are generally mild.
Azelaic acid:
A topical antiinflammatory used as an alternative to topical metronidazole. It is licenced for the relief of mild-to-moderate papulopustular acne of the face and the treatment of papulopustular rosacea. Some evidence suggests topical azelaic acid may have the benefit of not contributing to antimicrobial resistance when compared to topical metronidazole. Apply azelaic acid once or twice daily, for threeto-four months for maximum benefit.
Some 70-to-80 per cent of cases see symptom improvement to some degree within three-to-six weeks of commencement.
Side-effects of topical azelaic acid can include mild skin burning, stinging and irritation, especially on initial use. Tolerance to side-effects usually develops with ongoing use. Wash hands after each application to avoid irritating hands or inadvertently rubbing in the eyes. Avoid alcoholic cleansers, tinctures and astringents, abrasives and peeling agents when using azelaic acid to minimise irritation.
Comparing topical metronidazole to topical azelaic acid
No major differences in efficacy of topical metronidazole and topical azelaic acid have been noted in studies over the years. When comparing metronidazole to azelaic acid, metronidazole 0.75% gel was less effective than azelaic acid 15% gel (Skinoren) in reducing inflammatory lesions and erythema. Metronidazole 0.75% cream and azelaic acid 20% cream (Skinoren 20% cream, which is licenced in the UK but not in Ireland) induced significant and nearequal reduction in papules and pustules. Additionally, more satisfaction was reported with azelaic acid.
Topical Corticosteroids
Topical corticosteroids should be used to treat rosacea. While topical corticosteroids can give with short-term relief due to vasoconstrictive and anti-inflammatory action, they will aggravate symptoms over the following weeks. This is why topical corticosteroids are known as the ‘The Great Impostor’ when it comes to rosacea, as while they reduce inflammation and redness short-term, long-term use of topical corticosteroid actually causes rosacea-like symptoms.
Other topical treatments
Brimonidine gel 0.33% (Mirvaso) is relatively new to the market to reduce redness short-term in erythematous rosacea. It is more effective in treating flushing, but does not appear to be any more effective than metronidazole or azelaic acid for other rosacea symptoms. The possibility of rebound flushing can limit use of brimonidine gel.
Side-effects of topical
azelaic acid can include
mild skin burning,
stinging and irritation,
especially on initial use
The European Medicine Agency’s public assessment report in 2019 for Mirvaso stated that it “has not been systematically investigated” when compared to metronidazole or azelaic acid gel. While it does give relief, its effectiveness compared to more traditional treatments like metronidazole or azelaic acid is less proven, but more studies will help prove its effectiveness. Ivermectin cream (Soolantra) can improve papulopustular rosacea. Studies show ivermectin cream will produce partial to full clearance of rosacea lesions in 40-to-80 per cent of those with moderate-to-severe symptoms after three months of treatment. Studies indicated ivermectin is more effective than metronidazole cream and gave improved quality of life, reduced lesion counts, and less disease severity compared to metronidazole.
Oral rosacea treatments
NSAIDs
Oral medicines are reserved for rosacea that is resistant to topical treatments and for more with severe rosacea. Non-steroidal anti-inflammatory drugs (NSAIDs) will not cure the condition, but may relieve discomfort (or ‘soreness’) caused by rosacea and moderately ease erythema.
Oral antibiotics
Tetracycline antibiotics interfere with the inflammatory process that causes both acne and rosacea. They reduce rosaceaassociated erythema, papules, pustules, and eye symptoms. Tetracycline is effective at doses lower
than required for antimicrobial treatment, meaning the clinical benefit is not due to its antimicrobial effect, but
through the still unproven theory of its inhibition of metalloproteases. Metalloproteinases (MMPs), also called matrixins, are enzymes which function in the extracellular environment of skin cells and degrade both matrix and non-matrix proteins, such as collagen and elastin.
Doxycycline and minocycline are two tetracyclines effective against rosacea. Tetracyclines in lower doses, ie, 50mg daily are considered as effective as higher doses. Repeated courses of tetracyclines may be required but at low doses, antimicrobial resistance is not deemed an issue.
Recommended initial treatment regimens are:
Doxycycline 50mg, once daily, for sixto-12 weeks.
Minocycline 50mg, once daily, for sixto-12 weeks.
Gastrointestinal side-effects of tetracyclines can include heartburn, nausea, vomiting and diarrhoea. Photosensitivity, including photo-onycholysis, can occur when taking doxycycline. Photoonycholysis is a rare phototoxic reaction which causes the separation of the nail plate from the nail bed. Avoid prolonged exposure to UV light from the likes of sunlight when taking doxycycline; sunscreen is advised. Gastrointestinal adverse effects and photosensitivity are less likely with minocycline compared to doxycycline, though there is an increased risk of hepatitis drug-induced lupus erythematosus. Tetracycline antibiotics are teratogenic, so are contraindicated in women who are pregnant or breast-feeding. Oral contraceptives are advised in women of childbearing age. Doxycycline MR 40mg (Efracea MR 40mg) is licenced in the UK for rosacea with papulopustular lesions; it has fewer side-effects without being less effective than Doxycycline 100mg; however, it is not yet licensed in Ireland. Oral erythromycin may be prescribed for rosacea as an alternative to oral tetracyclines. Erythromycin is unlicensed for rosacea but is an effective antibiotic for papulopustular rosacea. Its use can be limited by gastrointestinal disturbance. Erythromycin at a dose of 250mg/ day is effective for rosacea when intolerant to tetracyclines or those where tetracyclines are contraindicated, including pregnant women. Clarithromycin is also sometimes used for rosacea where tetracyclines are contraindicated.
Isotretinoin
Low-dose oral isotretinoin is licensed for acne but not rosacea, but it is prescribed in an unlicensed manner by dermatologists as an alternative if oral antibiotics have been ineffective or not tolerated. The dose used for rosacea is approximately a quarter of that used to treat acne, meaning side-effects are minimised; however, the course needs to continue for many months or even longer.
There is good evidence to support its use with severe and persistent rosacea and in those with papulopustular and phymatous subtypes of rosacea. It is teratogenic, so female patients should use at least one effective form of contraception for one month before, during and one month after treatment has ceased. Isotretinoin and tetracyclines are contraindicated due to a higher risk of benign intracranial hypertension. Recommended isotretinoin regimen for rosacea is:
Isotretinoin, 0.1-0.3mg/kg/day for 12 weeks; followed by twice-weekly longterm dosing, if required. Side-effects of isotretinoin are numerous, but in low doses it is well tolerated. Side-effects include dry skin, lips, and eyes. Rarely, isotretinoin causes hepatic impairment, elevated serum lipid levels, pancreatitis and psychiatric events, including depression and suicide.
Drugs to reduce flushing in an unlicenced capactiy
Carvedilol, a non-selective beta-blocker with some alpha-blocking activity, may be prescribed to reduce flushing as an unlicensed indication. Carvedilol 6.25mg twice-daily is thought to be the effective dose for flushing in rosacea. As with all beta blockers, carvedilol is contraindicated with asthma, hypotension, or bradycardia.
Clonidine is
contraindicated with
severe bradyarrhythmia.
It is advised to
withdraw clonidine
slowly to prevent
rebound hypertension
Clonidine, an alpha2-receptor agonist, is sometimes prescribed as an unlicensed indication for rosacea to reduce flushing. Its effect on facial flushing is questioned by some experts. Low-dose regimens of clonidine are advised, ie, Clonidine, 25- to-50 micrograms daily. Clonidine is contraindicated with severe bradyarrhythmia. It is advised to withdraw clonidine slowly to prevent rebound hypertension. Calcineurin inhibitors, such as tacrolimus ointment and pimecrolimus cream, are again unlicensed but are only thought to give a small reduction in inflammation in severe rosacea. These unlicensed drugs should only be prescribed as a last resort when traditional licenced treatments have failed and symptoms are so severe that they are affecting the patient’s quality of life. They should only be prescribed under specialist dermatologist supervision.
Pharmacological treatment for ocular rosacea
Practice good eyelid hygiene and use ocular lubricants. Pharmacological treatment for ocular rosacea should only be considered after non-pharmacological treatments have been used without success. Evidence suggests oral tetracyclines (ie, doxycycline) and macrolides (ie, erythromycin) for one-to-three months improves tear film stability and increases meibomian secretions where ocular rosacea is severe.
Topical corticosteroids are best avoided and should only used for the short-term treatment of very severe inflammation or rosacea keratitis (best under supervision of an ophthalmologist); the long-term use of topical corticosteroids increases risk of glaucoma and cataracts.
Specialised treatments
Persistent telangiectasia that is not improved by conventional topical or oral therapies for rosacea may be treated with vascular laser or intense pulsed light treatment, with varying degrees of success in terms of reducing erythema and flushing. If these techniques are unavailable, cautery (use of mild electric current), diathermy (electrosurgery), or sclerotherapy (saline injections) may be beneficial. Where rosacea causes severe nose deformity (ie, rhinophyma), surgery or carbon dioxide laser may be used by dermatologists or plastic surgeons to reshape the nose.
References available upon request
Disclaimer: Brands mentioned in this article are meant as examples only and not meant as preference to other brands.
CONTRIBUTOR INFORMATION

Written and researched by Eamonn Brady (MPSI), owner of Whelehans Pharmacies in Mullingar
Tel 04493 34591 (Pearse St) or 04493 10266 (Clonmore). www.whelehans.inet. Eamonn specialises in the supply of medicines and training needs of nursing homes throughout Ireland. Email ebrady@whelehans.ie