A CLINICAL OVERVIEW OF PRESSURE SORES, INCLUDING CAUSES, PREVENTION, DIAGNOSIS AND TREATMENT.
Pressure ulcers are lesions caused by unrelieved pressure that results in damage to the underlying tissue. Generally, these are the result of soft tissue compression between a bony prominence and an external surface for a prolonged period of time. Pressure ulcers are among the most common conditions encountered in patients in hospital or requiring long-term institutional care. American studies have shown that pressure ulcers are also common among patients admitted to nursing homes, with reported rates ranging from 10-to-35 per cent.
For the purposes of this article, I will give a quick overview of causes, prevention and treatment; however, this only scratches the surface on an area in which there is very detailed research and treatment protocols, and the likes of tissue viability nurses have years of training and expertise to deal with what can be very complicated wounds.
CLINICAL MANIFESTATIONS AND DIAGNOSIS
Pressure ulcers are usually easy to identify by their appearance and location overlying a bony prominence. It is important to distinguish pressure ulcers from ulcers that result from diabetic neuropathy or arterial or venous insufficiency. They also may be confused with other conditions that cause redness of the skin, such as cellulitis. Superficial moisture-induced lesions, such as maceration (softening and whitening of skin) over a bony prominence, should not be labelled as ‘pressure ulcers’. Characteristics of lesions that need to be distinguished from pressure ulcers are:
- Diabetic neuropathic ulcers are seen in patients with diabetes who have peripheral neuropathy. The diabetic ulcer characteristically occurs on the foot, usually on the ball of the foot just behind the big toes or on the top of toes.
- Venous insufficiency ulcers are normally found on the inner part of the lower leg, usually just above the ankle. Approximately 70 per cent of all leg ulcers are venous ulcers. They can occur either on one or both legs and each leg may have more than one ulcer. They can range from painless, to extremely painful. These types of ulcers are common in people who have a history of leg and feet swelling. The ulcer usually presents itself as an open sore in an area that already typically exhibits a red-to-brown discoloration that has probably been present for some time. The area will also be swollen. Prior to the formation of the ulceration, the skin may have also been somewhat flaky and itchy as well. So long as there is no arterial disease, venous leg ulcers will benefit from elevation and compression dressings.
- Arterial ulcers occur as the result of arterial occlusive disease. Approximately 10 per cent of all leg ulcers are arterial ulcers. Feet and legs often feel cold and may have a whitish or bluish, shiny appearance. Arterial leg ulcers can be painful. Pain often increases when the legs are at rest and elevated.
CLASSIFICATION SYSTEM
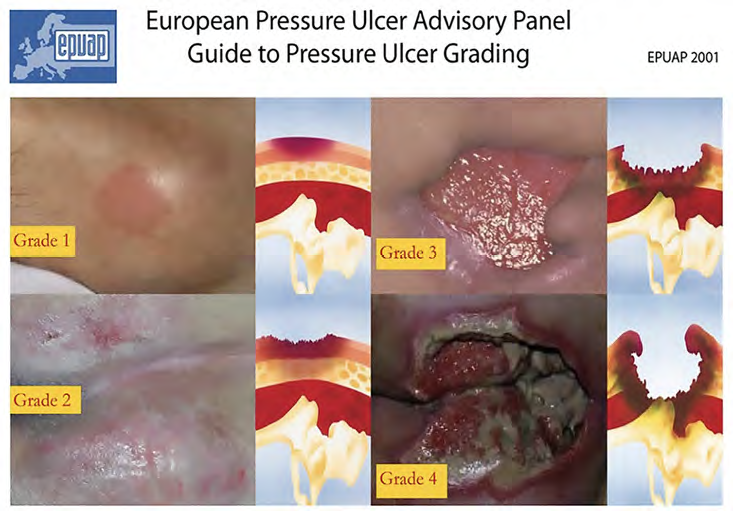
European Pressure Ulcer Advisory Panel (EPUAP) grading system (see Figure 1):
- Grade 1: Redness that does not whiten on touch. Discolouration of the skin, warmth, oedema, and hardness may also be used as indicators, particularly on individuals with darker skin, in whom it may appear blue or purple. Grade 1 may be more difficult to detect in those with dark skin tones.
- Grade 2: Partial thickness of skin loss involving epidermis, dermis, or both. The ulcer is superficial and presents clinically as an abrasion or blister. Surrounding skin may be red or purple. If bruising is visible at this stage, it can indicate deep tissue injury.
- Grade 3: Full thickness of skin loss involving damage to or necrosis of subcutaneous tissue. Subcutaneous fat may be visible, but tendon, muscle or bone are not exposed. Slough may be present.
- Grade 4: Extensive destruction, tissue necrosis, or damage to muscle, bone, or supporting structures with or without full thickness skin loss. Extremely difficult to heal and can lead to fatal infection.
Unstageable — Full thickness of tissue loss in which the base of the ulcer is covered by slough (yellow, tan, gray, green or brown) and/or eschar (tan, brown or black) in the wound bed.
Eschar often covers deep ulcers, making it difficult to determine whether lesions are stage 3 or 4. Until enough slough and/or eschar is removed to expose the base of the wound, the true depth, and therefore stage, cannot be determined.
CAUSES
EXTERNAL CAUSES
There are external factors that contribute to pressure ulcers. The four main external factors that lead to the development of pressure ulcers are pressure, shearing forces, friction, and moisture.
- Pressure: Pressure applied to the skin in excess of the arteriolar pressure (32mmHg) prevents the delivery of oxygen and nutrients to tissues, resulting in tissue hypoxia, the accumulation of metabolic waste products, and free radical generation. Pressures are greatest over bony prominences where weight-bearing points come into contact with external surfaces. Extensive deep tissue damage may occur with little or no evidence of superficial tissue injury. A deep necrotic wound may be the first evidence of pressure-induced injury, rather than a gradual progression of an ulcer from stages 1 through 4.
- Shearing forces: Shearing forces occur when patients are placed on an incline. Deeper tissues, including muscle and subcutaneous fat, are pulled downwards by gravity, while the superficial epidermis and dermis remain fixed through contact with the external surface.
- Friction: Friction occurs when patients are dragged across an external surface. This results in an abrasion with damage to the most superficial layer of skin. It is less likely to cause stage 3 and 4 ulcers than pressure.
- Moisture: Exposure to moisture in the form of perspiration, faeces, or urine may lead to skin maceration and predispose to superficial ulceration. There is little evidence regarding the magnitude of the contribution of moisture to pressure ulcer development.
PATIENT-SPECIFIC CAUSES
Patient factors that may contribute to pressure ulcer development include immobility, incontinence, nutritional status, circulatory factors, and neurological disease.
- Immobility: Immobility is the most important patient factor that contributes to pressure ulcer development.
- Incontinence: Urinary incontinence is frequently cited as a predisposing factor for pressure ulcers. Some studies suggest that incontinent patients have up to a five-fold higher risk for pressure ulcer development.
- Nutritional status: Among patients in hospital and care home settings, body mass index below 25kg/m2 is associated with greater risk of pressure ulcer development.
- Circulatory factors: The precise role of circulatory factors in pressure ulcer development must be further studied, although it appears likely that they will have a major role. Factors which can exacerbate or cause circulation issues include hypotension, dehydration, vasomotor failure, vasoconstriction secondary to shock, heart failure, or medications.
- Neurological diseases: Neurological diseases such as dementia, delirium, spinal cord injury, and neuropathy are important contributors to pressure ulcer development. This may be related to immobility, spasticity, and muscle contractions that are common in these conditions. Sensory loss is also common, suggesting that patients may not perceive pain or discomfort arising from prolonged pressure. Peripheral neuropathy due to diabetes is an example where pressure sores can occur due to sensory loss.
PREVENTION
The European Pressure Ulcer Advisory Panel made the following four points in relation to prevention of ulcers.
- Skin injury due to friction and shear forces should be minimised through correct positioning, transferring and repositioning techniques.
- Eliminate any source of excess moisture due to incontinence, perspiration or wound drainage.
- Reduce underlying risk factors, such as poor nutrition.
- Education and training, ie, mobility, positioning, skin care, use of equipment, for patients and their carers.
PRESSURE RELIEF
Patient positioning
Proper positioning of bed-bound individuals is recommended, including a regular turning and repositioning schedule, with particular attention to vulnerable tissue covering bony prominences such as the sacrum. Typically, a two-hour interval is recommended.
In addition to regular turning, the position of bed-bound patients is likely to be important. It is recommended that:
- Patients should be placed at a 30-degree angle when lying on their side to avoid direct pressure over the hip bone or other bony prominences.
- Pillows or foam wedges should be placed between the ankles and knees to avoid pressure at these sites when patients have no mobility at these areas.
- The heels require particular attention; pillows may be placed under the lower legs to elevate the heels, or special heel protectors can be used.
- The head of the bed should not be elevated more that 30 degrees to prevent sliding and friction injury.
Chair-bound patients may generate considerable pressures over the hip joints; they should be repositioned at least every hour with wheelchair push-ups or with tilting of the seat to reduce contact between the patient’s buttocks and the seat. Patients who are cognitively intact and can use their upper extremities can be trained to shift weight even more frequently, using monitoring devices as a reminder.
Support surfaces (mattresses) — these products can be classified as either non-powered, overlays, or powered.
Non-powered support surfaces (previously known as static) do not require electricity and consist of mattresses that are made of gel, foam, air, or water, or a combination of these. They work by distributing pressure over a wider body surface area.
Overlays are support surfaces designed to be placed on top of another support surface. Foam, air, or water overlays may be used for patients who can assume a variety of positions without bearing weight on the ulcer.
Powered or dynamic support surfaces require electricity to alternate air currents to regulate or redistribute pressure against the body. Examples include alternating pressure mattresses, low air loss beds, and air-fluidised mattresses.
For chair-bound patients, appropriate wheelchair cushions are recommended. Donut cushions should not be used, as they increase oedema and venous congestion and concentrate the pressure to surrounding tissue. The three main types of seat cushions include gel and foam seat cushions, non-powered adjustable cushions, and powered adjustable seat cushions.
MINIMISE IMMOBILITY
Encouraging patient mobility is key to the prevention of pressure ulcers. Several approaches may be helpful to minimise immobility, including:
- Immobilised patients may benefit from physiotherapy.
- Severe spasticity may be relieved by muscle-relaxant drugs, ie, Baclofen, or nerve block.
- Medications contributing to immobility, such as sedatives, should be stopped.
SKIN CARE
- Skin condition should be inspected and documented daily.
- Skin assessment should include skin temperature, colour, moisture status, and integrity. Any changes should be recorded as soon as they are observed.
- Keeping the skin clean and dry, while avoiding excess dryness and scaling, is the primary goal.
- Skin cleansing should be done with mild cleansing agents that minimise irritation.
- Hot water should be avoided.
- Vigorous massage over bony prominences should be avoided.
Cleansings should be done at regular intervals to minimise exposure to excess moisture due to incontinence, perspiration, or wound drainage.
MANAGEMENT
- Repositioning of the patient.
- Treatment of concurrent conditions which may delay healing, ie, poor circulation.
- Pressure-relieving support surfaces such as beds, mattresses, overlays, or cushions.
- Local wound management using modern or advanced wound dressings and other technologies.
- Patients with identified grade 1 pressure ulcers are at a significant risk of developing more severe ulcers and should receive interventions to prevent deterioration.
Pain relief
- Pain is often significant and disabling for those with pressure ulcers.
- Paracetamol may be sufficient, but patients often require stronger analgesia.
- Non-steroidal anti-inflammatory drugs may increase peripheral oedema and are inappropriate for patients with pressure ulcers, ie, Ibuprofen, Diclofenac.
- Opioid analgesics may be needed for moderate-to-severe pain.
- Topical local anesthetics such as lidocaine can provide numbness for a short period of time and can be useful for a specific procedure, but should not be used as the only method of pain relief.
- Wound cleansing and dressing techniques may need to be reconsidered if they are causing severe pain. In particular, adequate pain control should be provided for dressing changes and debridement.
- Patients may require referral to a pain clinic.
Nutrition
If oral intake is not adequate to ensure sufficient calories, protein, vitamins, and minerals, nutritional supplementation with enteral and parenteral nutrition (PEG feed) is recommended to correct deficiencies. Increased dietary protein intake promotes the healing of pressure ulcers. The protein target is usually 1.5g/ kg/day. Cubitan is an example of a high-energy, high-protein oral nutritional supplement (ONS) with wound-specific nutrients (arginine, vitamin C, zinc, vitamin E). It increases healing times of pressures sores in undernourished patients. However, it is important that oral nutritional supplements are reviewed regularly by a dietitian.
While high-protein ONS such as Cubitan have an important role in helping heal ulcers and other wounds, they should be discontinued promptly once the wound has healed.
Food is the best vehicle for appropriate nutrient consumption. According to the National Medicines Information Centre in St James’s Hospital, Dublin, no studies have yet determined the optimum usage of ONS in terms of the most appropriate patients, the optimum dose, and duration of use.
Non-steroidal anti-inflammatory drugs may increase peripheral oedema and are inappropriate for patients with pressure ulcers
Despite lack of evidence, ONS has a role in many circumstances; therefore, it is important to liaise with nutrition specialists such as dieticians before ONS can be recommended. For the added reason of the high cost of ONS to the State, the HSE also recommends that ONS is only commenced after the patient is assessed by a dietician.
Dressings
There is no conclusive research evidence to guide healthcare professional decision-making about which dressings are most effective in pressure ulcer management. However, professional consensus recommends that modern dressings (ie, hydrocolloids, hydrogels, foams, films, alginates, soft silicones) should be used in preference to basic dressing types, ie, gauze, paraffin gauze and simple dressing pads.
Grade 1 ulcers may be dressed with transparent films for protection, ie, Tegaderm, Opsite. Grade 2 pressure ulcers usually require an occlusive or semi-permeable dressing that will maintain a moist wound environment, ie, Comfeel Plus, Granuflex.
Ulcers with heavy exudate require an absorptive dressing to avoid build-up of chronic wound fluid that can lead to wound maceration and inhibit healing. An appropriate wound dressing can remove excess wound exudate while maintaining a moist environment to accelerate wound-healing. Dressings with absorptive qualities include alginates, ie, Kaltostat; foams, ie, Allevyn, Biatain; and hydrocolloids, ie, Aquacel, Comfeel, Granuflex.
Desiccated ulcers are dry ulcers that lack wound fluids which help promote heeling. Thus, pressure ulcer healing is promoted by dressings that maintain a moist wound environment while keeping the surrounding intact skin dry. Choices for a dry wound include hydrogels, ie, Granugel, Intrasite Gel; and hydrocolloids, ie, Aquacel, Comfeel, Granuflex.
Debridement
Necrotic tissue promotes bacterial growth and impairs wound-healing. Wound debridement may involve any of five approaches: Use of sharp dissection (take care when doing this on heels); mechanical debridement (wet-to-dry dressings); application of proteolytic enzymes; autolytic debridement under occlusive dressings (hydrocolloids or hydrogels); or biosurgery with sterilised maggots.
Infection control
- Reduce risk of infection and enhance wound healing by hand-washing, wound cleansing, and debridement. Protect from external sources of contamination, ie, faeces.
- If purulent material or foul odour are present, more-frequent cleansing and possibly debridement are required.
- When there are clinical signs of infection which do not respond to treatment, x-rays should be undertaken to exclude osteomyelitis and joint infection.
- Systemic antibiotics are required for patients with bacteraemia, sepsis, advancing cellulitis or osteomyelitis.
TOP TIPS FOR PREVENTION OF ULCERS
I focused on prevention of pressure sores already, but I finish with some everyday practical advice patients can use to prevent ulcers and pressure sores, many without the need for medical intervention. With the lower extremities (especially heel) and sacral area (buttocks) being two of the most common areas for pressure sores and ulcers, the tips and advice below are especially important in these areas, especially in patients prone to pressure sores, including diabetics and patients who are bed-bound. Diabetics are more prone to diabetic ulcers as well as pressure sores.
PREVENTING ULCERS AND PRESSURE SORES IN THE FEET OF DIABETICS
Check feet daily
Diabetics may have serious foot problems but feel no pain. Look for cuts, sores, red spots, swelling or infected toenails. Find a time (evening is best) to check feet each day. If trouble bending, use a mirror to help.
Wash feet daily
Wash feet in warm, not hot, water. However, do not soak feet, as this will cause the skin to get dry. Before bathing or showering, test the water to make sure it is not too hot. Use a thermometer (32-to-35oC is safe) or elbow. Dry feet well, taking care to dry between toes.
Keep feet moisturised
Rub a thin coat of skin lotion, cream, or petroleum jelly on the tops and bottoms of the feet. Do not put lotion or cream between toes, because this might cause an infection.
Do not overdo it
If using a pumice stone to smooth corns and calluses after bathing or showering, rub gently, in one direction only, to avoid tearing the skin. Do not cut corns and calluses. Diabetics should not use razor blades, corn plasters or liquid corn and callus removers, as they can damage skin.
Keep toenails trim
Cut toenails each week or when needed. Wash and dry the feet first. Trim toenails straight across and smooth them with an emery board or nail file. Do not cut into the corners of the toenail, as this can cause in-growing toenails. If eyesight is poor, if toenails are thick or yellowed, or nails curve and grow into the skin, have a chiropodist trim them.
Wear shoes and socks
Wear shoes and socks at all times. Do not walk barefoot — not even indoors — because it is easy to step on something and cause skin damage. Always wear socks, stockings, or nylons with shoes to help avoid blisters and sores. Socks that have no seams are best. Specially-designed socks for diabetics are ideal.
Avoid hot and cold
Always wear shoes at the beach or on hot ground and put sunscreen on the top of feet to prevent sunburn. Keep feet away from radiators and open fires and do not put hot water bottles or heating pads on feet. Check feet often in cold weather to avoid frostbite.
Keep the blood flowing
Put feet up when sitting. Wiggle the toes for five minutes, twice or three times a day. Move ankles up and down and in and out to improve blood flow. Do not cross your legs for long. Do not wear tight socks, elastic or rubber bands, or anything restrictive around your legs. Stop smoking, as it reduces blood flow to feet.
See a health professional
Diabetics should visit a chiropodist once every six months. Chiropodists are experts in foot health and should be the first stop if foot problems occur, especially in diabetics, as even minor issues can turn into serious problems very rapidly. Pharmacists and GPs can also help with foot problems.
GENERAL ADVICE TO PREVENT PRESSURE SORES
Relieve direct pressure
- Change position regularly and keep moving as much as possible.
- Change position at least every two hours.
- Stand up regularly to relieve pressure if sufficiently mobile.
- Ensure the carer repositions regularly where the patient cannot move independently.
- Use pressure-relieving mattresses and cushions (speak to an occupational therapist about these).
- Do not drag heels or elbows when moving in the bed or chair.
Skin care
- Keep the skin clean and dry.
- Keep skin well moisturised, especially after washing (as skin loses natural moisture when drying after washing).
- Avoid scented soaps, as they can be more drying.
- Avoid talcum powder, as it dries the skin’s natural oils.
General advice
- Ensure bedsheets are smooth and not wrinkled.
- Sheets should be cotton or silk-like fabric.
- Eat a well-balanced diet.
- Drink at least two litres of fluid a day (bearing in mind caffeine in tea and coffee is a diuretic and can exacerbate dehydration).
- Check skin daily for any changes like redness or irritation, especially in areas like the buttocks or heels that are more prone. Use a mirror to check hard-to-reach areas or ask a loved one or carer to check these areas.
- Inform your doctor or nurse of any skin changes or discomfort as soon as possible, no matter how minor; even slight redness, as this is the first sign of an ulcer developing.
References available upon request
Disclaimer: Brands mentioned are meant as examples only and not meant as preference to other brands.
CONTRIBUTOR INFORMATION

Written by Eamonn Brady MPSI (Pharmacist). Whelehans Pharmacies, 38 Pearse St and Clonmore, Mullingar. Tel 04493 34591 (Pearse St) or 04493 10266 (Clonmore). www.whelehans.ie. Eamonn specialises in the supply of medicines and training needs of nursing homes throughout Ireland. Email ebrady@ whelehans.ie







