Whilst covid has dominated the healthcare landscape since last year, the perennnial problem of coughs, colds and flu has not gone away
Cold or influenza (flu) are caused by viruses and so have no cure, but the symptoms can be relieved by over-the-counter remedies. These symptoms include runny/blocked nose, sneezing/coughing, aches and pains, high temperature and sore throat. The flu comes on suddenly, whereas a cold develops over several hours.
Flu is a much more ‘hard-hitting’ illness than a cold and will usually leave the sufferer confined to bed for a few days (more about flu symptoms later in this article). The symptoms of a cold, while unpleasant, usually allow the sufferer to continue his or her normal daily activities; however, with Covid-19 in our community, movements must be restricted until Covid-19 is ruled out by a PCR test. Symptoms of a cold are generally confined to the head, whilst a patient with the flu will feel sick all over.
The treatment for both colds and flu are similar. Colds and flu symptoms generally last a maximum of seven days and need no specific treatment other than painkillers for aches, pains and temperature and simple measures, such as decongestant rubs or vaporisers. Antibiotics are of no benefit, as both colds and flu are caused by viruses.
COVID-19 MUST ALWAYS BE ASSUMED
Covid-19 has complicated things, as when people get cold- or flu-like symptoms, it first must be considered if it is Covid-19. If getting a PCR test, the person should self-isolate until they get a negative result. Even if the Covid-19 result is negative, best practice is that the person still restricts movements until 48 hours after the cold/flu-like symptoms ease.
Covid-19 is a coronavirus like the common cold, but the symptoms can be a lot more severe, especially if not vaccinated, and Covid-19 has specific symptoms that differ from the common cold, like loss of taste and smell. While the symptoms of influenza can be similar to Covid-19, inf luenza is a completely unrelated virus.
Reduction in coughs, colds and flu due to public health restrictions Last flu season (2020/21), there were no recorded cases of influenza in Ireland. This was attributed to the public health measures to reduce the spread of Covid-19, ie, movement restrictions, social distancing, mask-wearing, and better hand hygiene. Similarly, the Covid-19 public health measures reduced incidences coughs and colds.
The best indicator of this is figures released by retail analyst Kantar in March 2021, showing that sales of cold and flu treatments fell by 55 per cent in the previous 12 weeks, while cough syrup sales fell by 60 per cent in the same period.
Some figures show that some cold and flu remedy sales fell by over 70 per cent in 2020; this is despite ‘panic buying’ and ‘hoarding’ of cold and flu remedies by people at the start of the pandemic in March 2020.
However, since the end of summer 2021 and as public health measures have eased, as well as a resurgence of Covid-19, there has also been a resurgence in coughs and colds and general respiratory viral infections, with respiratory syncytial virus (RSV) being a particular problem in children in recent months.
COLD AND FLU TREATMENT
The age of the patient will influence choice of products.
- Runnt nose and congestion are both treated by decongestants.
- Sneezing is treated by an antihistamine.
- Cough may be due to irritation or post-nasal drip. An expectorant mixture can help.
- Headaches are due to inflammation of the sinuses and nasal passages muscular or joint pain is common —this will need a painkiller.
- Sinus pain worsens on leaning forward or lying down and may develop into an infection.
- High temperature is more common in the flu than with a cold — paracetamol is very useful to bring down a high temperature.
- Sore throat is usually the first sign of a cold, and one of the common OTC sore throat lozenges will help.
PRECAUTIONS
Many cold and flu remedies contain several drugs, so anyone on prescription medication should speak to the pharmacist. Anyone who is pregnant, has heart disease or lung disease or the very young or old should also be seen by the pharmacist.
So, for example, if someone suffers with high blood pressure, it is best to avoid many cold and flu remedies which contain decongestants, as these products tend to raise blood pressure.
Asthmatics and people with stomach complaints such as stomach ulcers should avoid products which contain aspirin and non-steroidal anti-inflammatories (NSAIDs) like ibuprofen. This is because aspirin and NSAIDs can trigger asthma attacks in some asthmatics and irritate stomach ulcers. There are a vast number of preparations available for the treatment of cold and flu symptoms, some of which are combination preparations and may be capable of treating many symptoms at once.
COUGH
Essentially, there are two types of cough; a dry or a chesty cough. During a cold, a cough is often caused by a nasal drip irritating the back of the throat. Chesty coughs occur when mucus (also called phlegm or catarrh) builds up in the airways and the cough occurs so the body can clear the mucus. Chesty cough mixtures with an expectorant like guaifenesin or carbocisteine liquefy the catarrh so that it can be coughed-up easier.
There are other cough mixtures that cause drowsiness, which can be used at night to help sleep. Sugar-free versions of cough mixtures are available for diabetics. Dry cough mixtures contain ingredients such as pholcodeine, codeine and dextromethorphan. Dry cough mixtures come in drowsy or non-drowsy versions. There are also cough mixtures available that contain decongestants which can be effective with a congested head as well as a cough.
SELF-HELP FOR COUGHS
Stop smoking
If you are determined to continue smoking, at least stop for the duration of the cough. This gives the lungs an opportunity to try to clear the infection. When you stop smoking, you will find you cough more for a few weeks as your lungs clear the tar that coated your lungs while you smoked.
Steam inhalations
Steam inhalations can be useful, particularly in productive (chesty) coughs. Simply putting hot steaming water (not boiling) in a basin, putting a towel over one’s head and inhaling the steam can accelerate the clearing of catarrh. The steam helps to liquefy lung secretions and the warm, moist air is comforting. Adding a little eucalyptus to the steaming water is a favourite of some people.
Increase fluid intake
Maintaining a good fluid intake helps to hydrate the lungs. Hot drinks like hot lemon and honey provide a soothing
and comforting effect.
Could the cough be due to
blood pressure medication?
A type of blood pressure medication can cause a persistent dry cough in some people. The class of drug that causes this cough is ACE inhibitors. Examples include ramipril, perindopril, and lisinopril. About 10-to-15 per cent of people who use this class of blood pressure medication experience a dry cough. The incidence of cough appears to be higher in women.
It is a persistent dry cough, which is worse when lying down and generally does not start for 24 hours after starting an ACE inhibitor. If the dry cough occurs, the doctor will need to change to another drug, ie, an angiotensin 2 inhibitor. The cough will subside once the ACE inhibitor is stopped.
COUGHS IN CHILDREN
Coughs are more common during school term and are caused by common viruses, which are commonly passed from child-to-child in school. Whilst rarely serious, coughs and colds are an inconvenience and lead to many missed school days. Some prevention tips help prevent coughs and colds.
Examples, which have become more common due to Covid-19, include ensuring your child washes their hands regularly and properly, especially after touching their nose or mouth and before handling food. Teach them to always sneeze and cough into tissues to prevent spreading infection. Whilst less likely in this era of Covid-19, sharing cups and utensils is a common way to spread colds and flu.
Chesty coughs are especially common as kids return to school. An antibiotic is rarely needed. Only 20 per cent of chest infections are bacterial, so antibiotics are ineffective in most cases.
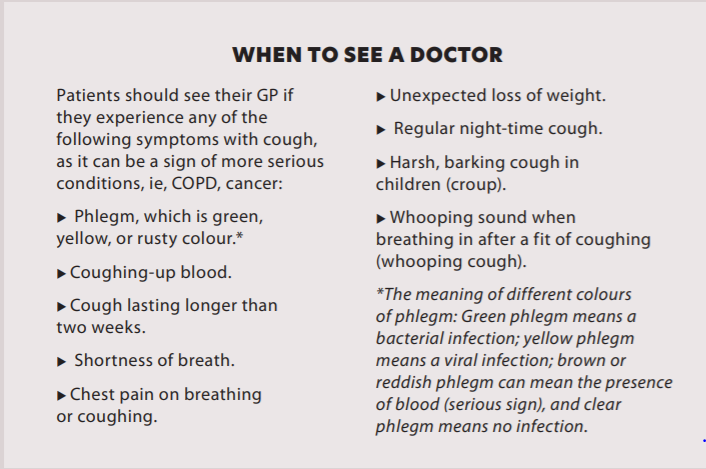

GUIDELINES FOR COUGH AND COLD REMEDIES FOR CHILDREN
Guidelines introduced in 2011 restricted the sale of cough and cold remedies to children aged under six. The Health Product Regulatory Authority (HPRA) brought these guidelines out not because of any safety concerns in children under six, but because they recognised that coughs and colds in children are frequent and normally self-limiting, and there is no real evidence to support the use of these products in children under six.
So, due to these guidelines, pharmacies can no longer sell products containing cough suppressants, decongestants or antihistamines to undersixes. Common OTC remedies can no longer be given to children under six. For a child under six, the best advice is rest and drink plenty of fluids. Most coughs and colds in children under six will pass quickly but if is not improving or there is signs of a bacterial chest/ nasal infection (green mucus is a sign), an antibiotic may be needed, however over 80 per cent of coughs and colds are viral, so no antibiotic is needed.
Saline drops or spray are a good and safe option to clear sinuses in children over six. Decongestant rubs or drops that can be put on the child’s chest or hankie beside the bed can be comforting for the child. Paracetamol liquid is still recommended for high temperature for under-sixes.
For children over six, there are many
OTC products and there is no one that stands out as best. Always double-check the dose before giving, as there are different doses for different ages.
PREVENTION
As so many different viruses can cause the common cold, there is no vaccination against it. Some prevention tips are:
- Wash your hands regularly and properly, most importantly after touching the nose or mouth and before handling food.
- Always sneeze and cough into tissues to prevent spreading infection.
- Do not share cups or kitchen utensils with others. Use your own cup, plates, and cutlery.
INFLUENZA
Influenza (flu) is a highly infectious acute respiratory illness caused by the influenza virus. It can affect people of any age.
The seasonal flu vaccine (flu jab) protects against four strains of flu virus. These are the strains most likely to be circulating this flu season, based on WHO evidence of virus circulation in the Southern Hemisphere in the previous flu season.
The four strains in the 2021/22 vaccine are:*
- an A/Victoria/2570/2019 (H1N1) pdm09-like virus
- an A/Cambodia/e0826360/2020 (H3N2)-like virus.
- a B/Washington/02/2019 (B/Victoria lineage)-like virus.
- a B/Phuket/3073/2013 (B/Yamagata lineage)-like virus.
The flu vaccination is available through GP surgeries, local pharmacies, and some workplaces.
SYMPTOMS OF FLU
Symptoms of flu include sudden fever, chills, headache, muscle pain, sore throat, non-productive dry cough, exhaustion, and weakness. Flu characteristically causes a temperature of 38-to-0°C that lasts three-to-four days.
DIFFERENCE BETWEEN COLD AND FLU
A cold will develop slowly over a few days, with symptoms like a sore throat and a blocked or runny nose. The symptoms of flu hit you suddenly and severely with symptoms like fever and muscle aches. Often, people suffering from a bad cold wrongly believe they have flu. Flu causes extreme exhaustion, muscle aches, severe sweats and leaves you so weak that you will not be able to get out of bed. Work and other normal routines are not possible with flu.
COMPLICATIONS OF FLU
Most people recover from flu in two-to seven days, but in some it can last for up to two or three weeks. Flu can be severe and can cause serious illness and death, especially in the very young and in the elderly. Serious respiratory complications can develop, including pneumonia and bronchitis. Older people and those with certain chronic medical conditions are at particular risk of these complications.
Pregnant women and women up to six weeks after giving birth have also been found to be at increased risk of the complications of flu. Eighty-to-90 per cent of reported deaths from influenza occur in the elderly, mainly from bacterial pneumonia (200 deaths per year in Ireland), but also from the underlying disease.
Social distancing, mask-wearing and increased uptake in flu vaccines meant there was no incidence of influenza in the 2021/22 flu season, as the flu virus had less chance to spread. With restrictions eased, influenza figures for the 2021/22 season are likely to return to pre-Covid levels.
THOSE CONSIDERED
MORE ‘AT-RISK’ FROM FLU
Some people are more at risk of getting complications if they catch flu. People can get the HSE flu vaccine for free if they:*
- Are 65 years of age and over.
- Are pregnant.
- Are a child aged two-to-17 years.
Are an adult or child aged six months
or older at increased risk for flu-related
complications, including:
- Those with long-term conditions:
- Chronic heart disease, including acute coronary syndrome.
- Chronic liver disease.
- Chronic renal failure.
- Chronic respiratory disease, including COPD, cystic fibrosis, moderate or severe asthma, or bronchopulmonary dysplasia.
- Chronic neurological disease, including multiple sclerosis, hereditary and degenerative disorders of the central nervous system.
- Diabetes mellitus.
- Haemoglobinopathies.
- Morbid obesity, ie, body mass index (BMI) over 40
- Immunosuppression due to disease or treatment (including treatment for cancer).
- Children with a moderate-to-severe neurodevelopmental disorder, such as cerebral palsy.
- Children on long-term aspirin therapy
- Those with any condition that can compromise respiratory function (ie, spinal cord injury, seizure disorder or other neuromuscular disorder), especially those attending special schools or day centres.
- Were born with Down syndrome.
- Live in a nursing home or other long-term care facility.
Some people should get the vaccine to protect themselves, their families and those they care for. These include:
- Those who work in healthcare.
- Only household contacts or carers of people who have an underlying chronic health condition or have Down syndrome are eligible to receive an influenza vaccine. A carer is described as someone who is providing an ongoing significant level of care to a person who is in need of care in the home due to illness or disability or frailty.
- People who are in regular contact with pigs, poultry or waterfowl should get the flu vaccine.
Not all household contacts are eligible for the free flu vaccine. NIAC has recommended the flu vaccine only for
household contacts of people with certain long-term medical conditions or people who have Down syndrome.
The following household contacts are not recommended the flu vaccine.
Household contacts of:
- People aged 65 and over
- Pregnant women
- Children aged two-to-17.
- Healthcare workers.
- Carers
Household contacts that are not in a recommended group themselves cannot avail of the free flu vaccine provided through the HSE programme and instead, they must source the flu vaccine privately, should they wish to get vaccinated.
Bear in mind, the flu vaccine is not free for medical card or doctor visit card-holders unless they are part of the ‘at risk’ groups mentioned above.
FLU VACCINES AVAILABLE
FOR THE 2021/22 SEASON
The 2021/22 HSE seasonal vaccination programme offers three vaccines:
- The Quadrivalent Influenza Vaccine (split virion, inactivated) manufactured by Sanofi Pasteur for people with longterm conditions.
- The adjuvanted Quadrivalent Influenza Vaccine (aQIV) called Fluad Tetra and is manufactured by Seqirus for people aged 65 years and over.
- The Fluenz Tetra nasal spray suspension Influenza vaccine (live attenuated, nasal) manufactured by AstraZeneca AB for children aged two-to-17 years.
Pharmacies must purchase flu vaccines (ie, Influvac Tetra) from wholesalers to administer to private patients who are not in the above risk groups ie, patients who must pay privately for the flu vaccine. The earlier the patient gets the vaccine the better as they can take up to two weeks to work.
The actual expiry date of all this season’s adult flu vaccines (once stored correctly in a fridge) is 06/22, while the expiry date of the Fluenz Tetra 2021/22 nasal spray for children is 17/12/21.
FLU VACCINE SIDE-EFFECTS
There may be a mild fever and aching muscles for a couple of days after having the vaccine. The arm where the vaccine was given may also be a bit sore. Serious side-effects of the flu vaccine are very rare. There is no aluminium, thiomersal, mercury, gelatin or porcine gelatin in the Quadrivalent Inactivated Influenza vaccine used in the 2021/22 campaign.
FLU VACCINE FOR CHILDREN
Children are more likely than adults to get severe complications of flu. Children who are sick with flu miss days in crèche, childcare and school. They also miss out on their usual activities, such as hobbies and sports. Children aged two-to-12 can now get the nasal flu vaccine for free.
The flu vaccine will help protect a child against flu and reduce the spread of flu to others, for example, their brothers and sisters, parents, and grandparents.
The vaccine is given as a single spray in each nostril of the child’s nose. The child can breathe normally while getting the vaccine. There is no need to take a deep breath or sniff. The vaccine is not painful and is absorbed quickly. It will work even if the child has a runny nose, sneezes, or blows their nose after the vaccination.
Most children need only one dose of the vaccine each year. Some children with chronic health conditions like chronic heart or lung conditions may need two doses. The doses are given four weeks apart for these high-risk children if they have never had a flu vaccine.
SIDE-EFFECTS OF
THE NASAL FLU VACCINE
The most common side-effects are mild
and include:
- A runny or blocked nose.
- Headache.
- Muscle aches.
Some children get a fever (temperature) after the vaccine. It is usually mild and goes away on its own. If the child has a fever or a headache, paracetamol or ibuprofen can help. Aspirin, or any medicines that contain aspirin, should never be given to children unless prescribed by a doctor (due to risk of Reye’s syndrome). This is especially important in the four weeks after getting the flu vaccine.
Serious side effects such as a severe allergic reaction are rare. There is no evidence that you can catch flu from the nasal flu spray.
*Reference: HSE 2021/22 flu vaccine update Thanks to the HSE for flu vaccine 2021/22 updates. Other references on request. Disclaimer: Brands mentioned in this article are meant as examples only and not meant as preference to other brands.

Written and researched by Eamonn Brady (MPSI), owner of Whelehans Pharmacies in Mullingar Tel 04493 34591 (Pearse St) or 04493 10266 (Clonmore). www.whelehans.inet. Eamonn specialises in the supply of medicines and training needs of nursing homes throughout Ireland. Email ebrady@whelehans.ie