Damien O’Brien MPSI outlines the role of community pharmacists in supporting the healthy development of infants
Introduction
An infant is typically defined as a child from birth to 12 months of age. This period is characterised by rapid physical growth, cognitive maturation, and social development. Infant care extends beyond the management of illness and encompasses a broad spectrum of practices aimed at supporting healthy development, preventing disease, and promoting overall wellbeing during this early stage of life.
Adequate nutrition, safe sleep practices, hygiene, immunisation, appropriate medicine use, and a secure caregiving environment all contribute to optimal outcomes during this formative period.
Community pharmacies occupy a uniquely accessible position within the Irish healthcare system, often serving as the first point of contact for parents concerned about their infant’s health.
Pharmacists play a crucial role in supporting parents by providing guidance on various aspects of infant care, including medication safety, common health conditions, nutrition, immunisation schedules, and preventive healthcare measures. Through evidence-based guidance and supportive communication, pharmacists contribute significantly to promoting infant health during the first year of life.
This article explores key components of infant care commonly encountered in community pharmacy practice in Ireland, including principles of good infant care, nutritional and feeding support, the infant immunisation schedule, and common infant conditions presenting in pharmacy practice. The safe use of medication and recognition of red flag symptoms are also discussed.
Good infant care practices
Good infant care practices provide the foundation for healthy growth and development during the early stages of life. Maintaining good hygiene is particularly important in infancy. Regular hand-washing, particularly before feeds or after nappy changes, is central to reducing infection risk.
Appropriate nappy care, including frequent changes and the use of barrier preparations when required, helps preserve skin integrity and reduces the risk of dermatitis and infection. Gentle bathing practices should be encouraged, avoiding excessive washing and using mild, unscented products.
Safe sleep guidance is important to promote healthy development and reduce the risk of sleep-related harm. Infants should be placed on their back in a safe cot with a clear and uncluttered sleep space. Environmental and household safety also play a significant role in infant wellbeing.
Maintaining appropriate room temperature, avoiding exposure to tobacco smoke, and ensuring safe storage of medicines and household products are important preventive measures. Finally, regular interaction and responsive caregiving support early emotional and social development in infants.
Nutrition and feeding support
Adequate nutrition during infancy is fundamental to optimal growth, development, and immune function. Pharmacists can offer guidance on many aspects of infant nutrition, including breastfeeding, formula feeding, the introduction of solid foods, and the management of common feeding concerns. Providing balanced, evidence- based, and non-judgemental guidance while supporting parental choice is essential in this area.
Breastfeeding is recommended as the optimal source of nutrition for infants where possible. It provides complete nutritional requirements in early life while also offering immunological protection through the transfer of maternal antibodies. Breastfeeding is associated with reduced rates of infection and gastrointestinal issues in infants. Maternal benefits include reduced risk of certain chronic health conditions and enhanced bonding between mother and baby.
Breastfed infants are recommended to receive vitamin D supplementation of 5?g (200IU) daily during the first year of life, representing an important counselling point for pharmacists. Pharmacists can provide support with latch techniques, nipple care, and general lactation advice, while recognising when referral to additional breastfeeding support services may be necessary. Medication safety during breastfeeding is another common area of enquiry, with pharmacists well placed to advise on appropriate medicine use during lactation.
Infant formula provides a safe and nutritionally complete alternative to breastfeeding. Pharmacists may counsel caregivers on appropriate formula selection and help identify possible signs of feeding intolerance that may require further assessment. Guidance on the correct preparation and storage of formula, including appropriate water temperature and safe handling practices, is essential to minimise infection risk. Weaning and the introduction of solid foods are important developmental stages.
Pharmacists can offer advice on suitable food choices and address concerns such as choking risk, food intolerance, colic, reflux, flatulence, and constipation. Pharmacist counselling should emphasise reassurance alongside practical feeding advice, helping caregivers recognise normal feeding patterns while remaining alert to warning symptoms that may warrant further medical assessment.
Immunisation schedule
Immunisation is a safe and effective public health intervention designed to protect infants from serious infectious diseases during a period of increased vulnerability. Due to immature immune systems, early vaccination plays a
Safe sleep guidance is important to promote healthy development and reduce the risk of sleep-related harm
critical role in reducing morbidity and mortality associated with preventable illnesses. Pharmacists play an important role in educating caregivers about the importance of vaccination. This includes addressing common parental concerns, correcting misinformation, explaining vaccine benefits clearly, and discussing vaccine safety monitoring processes.
Pharmacists should counsel caregivers on expected adverse effects, with mild fever, irritability, and local injection-site discomfort among the most common. Guidance can also be provided on the appropriate management of these symptoms, including weight-based dosing of paracetamol where appropriate. By promoting adherence to the recommended immunisation schedule and providing evidence-based reassurance, pharmacists contribute significantly to infant health and wider community protection.
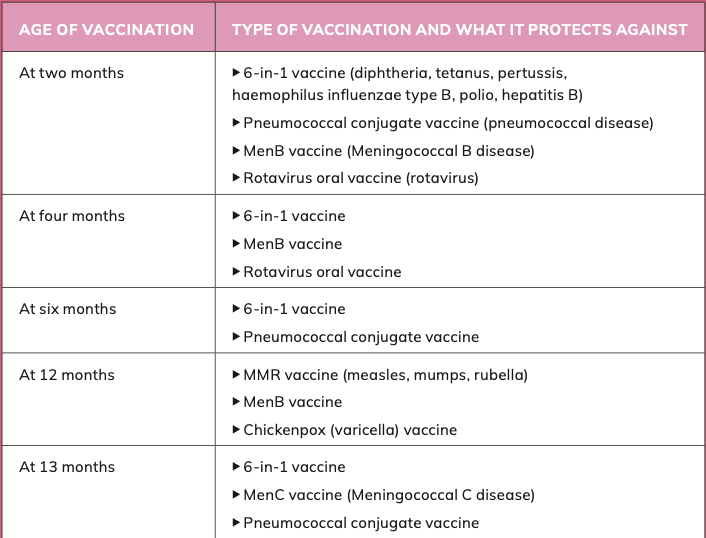
In Ireland, childhood vaccines are delivered through the National Immunisation Programme according to a structured schedule during early life. Timely completion of the schedule ensures optimal immune protection during early infancy, when the risk of severe infection is highest. Routine vaccinations are administered at approximately two, four, six, 12, and 13 months of age, protecting against a wide range of serious illnesses. The immunisation schedule is outlined in table 1.
Common infant conditions
A wide range of minor conditions affect infants, many of which are self-limiting but can cause significant parental concern. Pharmacists can assist in managing these common presentations through clinical advice and appropriate over-the-counter treatment options, while recognising situations where medical referral may be required.
Infection
Infections are among the most common cause of illness during infancy. They may occur at any age but are particularly concerning in young infants due to their underdeveloped immune systems. Infections may have a viral, fungal, or bacterial origin.
Fungal infections
Fungal infections, particularly oral candidiasis and candidal nappy rash, are frequently encountered in infancy. Early recognition and appropriate topical treatment can prevent progression and reduce discomfort. Symptoms of oral candidiasis include white plaques in the mouth, a white coating on the tongue, cracked corners of the mouth, and reluctance to feed. Treatment options include oral miconazole gel or nystatin oral suspension. Miconazole may be used in infants older than four months, while nystatin can be used from birth. Both treatments are typically applied four times daily, ensuring the medication remains in contact with affected areas for as long as possible. Caregivers should be advised to apply small amounts carefully to reduce the risk of choking.
Ensuring thorough cleaning and drying of the nappy area can reduce the risk of candidal nappy rash. A protective barrier cream may help prevent skin irritation, while a topical antifungal treatment, such as clotrimazole, can be used when infection is present.
Viral infections
Viral infections are also common in infants. While many viral illnesses are mild and self-limiting, some can lead to more serious complications in young infants. Prevention involves good hygiene practices, vaccination, and avoiding close contact with individuals who are unwell.
Hand, foot, and mouth disease is a common viral illness affecting infants and young children. Initial symptoms include sore throat, fever, irritability, and loss of appetite. Mouth ulcers and a rash on the hands and feet often appear after a few days. The condition is usually self- limiting, and symptoms may be managed with paracetamol where appropriate, alongside supportive care focused on maintaining hydration.
Infants are particularly vulnerable to respiratory viral infections, ranging from the common cold to more severe lower respiratory tract illness. The common cold is frequently caused by viruses such as rhinoviruses and adenoviruses and typically presents with a runny nose, cough, sneezing, mild fever, and irritability. Influenza can cause more severe illness in infants, particularly those under six months of age, with symptoms including fever, cough, sore throat, body aches, reduced feeding, and irritability. Management is primarily supportive, focusing on maintaining hydration, relieving nasal congestion, controlling fever, and monitoring for signs of clinical deterioration.
Respiratory syncytial virus (RSV) is a respiratory virus that is a leading cause of bronchiolitis and pneumonia in infants. Most infections are self-limiting and present with symptoms such as nasal congestion, cough, fever, and wheezing, with most infants recovering within two weeks without the need for further treatment. In more severe cases, infants may develop respiratory distress requiring medical assessment.
RSV infection can lead to respiratory failure and hospitalisation in severe cases, particularly among premature infants and those with underlying medical conditions. There is no specific antiviral treatment, and supportive care remains the mainstay of management. There is no routine active RSV vaccine currently used in infants — however, nirsevimab is a monoclonal antibody that provides passive immunity and has been introduced into Ireland’s immunisation programme for eligible infants. A single dose provides protection for approximately 150 days of life, corresponding to the period of highest risk for severe RSV infection.
Bacterial infections
Bacterial infections cause a wide range of illnesses, ranging from mild, self-limiting conditions to severe, life-threatening diseases. Clinical presentation varies depending on the organism and site of infection, necessitating a tailored treatment approach. Urinary tract infections (UTIs) result from bacterial infection of the urinary tract and may present in infants with fever, irritability, poor feeding, vomiting, or malaise. Antibiotic therapy should be guided by urine culture and sensitivity testing, with treatment options including amoxicillin, cefalexin, trimethoprim, or nitrofurantoin where appropriate. Pneumonia and bronchitis may also occur secondary to bacterial infection, presenting with cough, fever, lethargy, and difficulty breathing, with severe cases potentially progressing to respiratory distress and hospitalisation. Management typically involves appropriate antibiotic therapy alongside supportive care.
Colic
Colic is a common condition affecting up to 20 per cent of infants and is characterised by excessive and prolonged periods of unexplained crying in an otherwise healthy infant. Other symptoms may include clenching of fists, restlessness, and redness in the face. Symptoms typically peak during the first few months of life. Although colic is distressing for parents, it is self- limiting and usually resolves with time. Management strategies may include winding techniques, use of anti-colic bottles, and, in some cases, simethicone drops, although evidence supporting pharmacological treatments remains limited. Reassurance, parental support, and coping strategies therefore remain central to management.
Reflux
Gastroesophageal reflux is common in infancy due to physiological immaturity
Features such as poor weight gain, persistent distress or feeding refusal should prompt referral for further assessment
of the lower oesophageal sphincter, affecting up to 40 per cent of infants. Non-pharmacological measures, including upright positioning after feeds, and avoiding overfeeding, often lead to improvement in symptoms.
Features such as poor weight gain, persistent distress or feeding refusal should prompt referral for further assessment. Reflux typically improves and resolves before 12 months of age without the need for pharmacological treatment. Proton pump inhibitors (PPIs) and histamine-2 (H2) receptor antagonists may be considered under medical supervision if other options fail.
Teething
Teething commonly occurs from approximately six months of age and may present with irritability, drooling, and gum discomfort. Mild temperature elevation may occur; however, significant fever or systemic illness should not be attributed solely to teething. Management focuses on non pharmacological comfort measures such as chilled teething rings and gentle gum massage, while paracetamol may be considered if required.
Medicines use in infants: Safety and counselling
The safe use of medicines in infancy requires particular care, as infants differ significantly from adults in both pharmacokinetics and pharmacodynamics. Immature hepatic metabolism, renal function and differences in body composition can influence drug absorption, distribution, metabolism and excretion. Weight-based dosing is the cornerstone of safe medicine use, and caregivers should be encouraged to use the infant’s most recently recorded weight whenever possible. Demonstration of appropriate measuring devices, such as oral syringes and measuring spoons, is essential as dosing errors are common. Certain over-the-counter preparations are not recommended for young infants due to limited efficacy and potential safety concerns, and pharmacists should guide caregivers towards safe and evidence- based options. Counselling on safe storage of medicines is also vital to reduce the risk of accidental ingestion and poisoning.
The role of the pharmacist
Pharmacists play a central role in educating and supporting parents and caregivers across all aspects of infant care through the provision of accessible, evidence-based guidance. As highly accessible healthcare professionals, pharmacists are frequently the first point of contact for parental concerns, allowing timely intervention, reassurance, and appropriate clinical advice. A key component involves providing clear, evidence-based information on preventive healthcare measures, such as vaccinations.
Pharmacists also support caregivers in the assessment and management of common infant ailments and promote the safe use of medicines through counselling on appropriate product selection, accurate weight- based dosing, administration techniques, and potential adverse effects. Importantly, pharmacists are well placed to recognise red flag symptoms requiring referral to a GP or emergency services. Through their accessibility, clinical expertise and supportive communication, pharmacists make a significant contribution to infant health while also providing reassurance and confidence to parents and caregivers.
References upon request