Eamonn Brady MPSI provides a clinical synopsis of the causes, symptoms and treatment of seborrhoeic dermatitis
Introduction
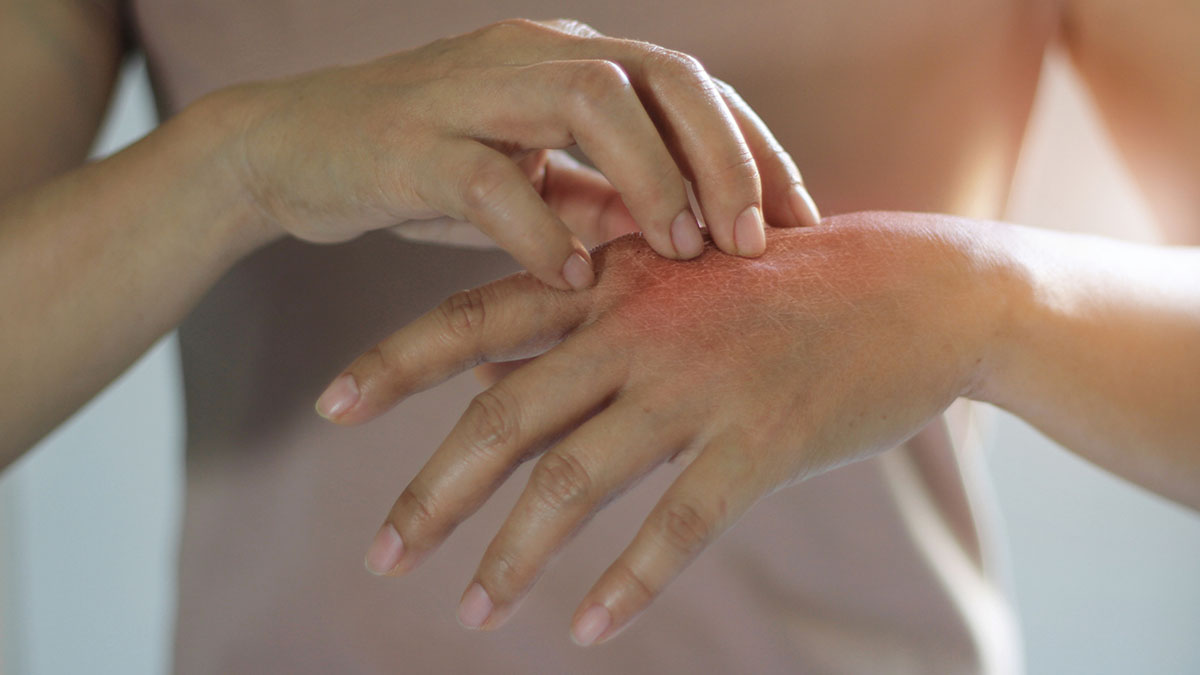
The term ‘seborrhoeic dermatitis’ is derived from the distribution of this disorder, in which erythematous, scaly patches develop in areas that are rich in sebaceous glands, such as the scalp, face, and upper trunk. The term ‘seborrhoea’ refers to excess oil secretion, although this finding is not uniformly present in patients with seborrhoeic dermatitis.1,2 It is more likely to affect men than women.
It is commonly aggravated by changes in humidity, changes in seasons, trauma (ie, scratching), or emotional stress. The usual onset occurs with puberty. It peaks at age 40 years and is less severe in older people. Approximately 1-to-3 per cent of adults suffer from seborrhoeic dermatitis.3 Dandruff is a mild form of seborrhoeic dermatitis and is estimated to affect 15-to-20 per cent of the population.
Cause
The cause of seborrhoeic dermatitis is unknown. There is evidence that malassezia fungi may have an influence.4 Malassezia are lipid-dependent organisms which are normally present on the skin surface. However, in patients suffering from seborrhoeic dermatitis, there is evidence of an abnormally high level of malassezia fungi on the skin, which leads to an inflammatory response.5 This theory is supported by the fact that seborrhoeic dermatitis responds to antifungal treatment.
Symptoms
Seborrhoeic dermatitis presents as erythema and scale, with some itch. Seborrhoeic dermatitis most commonly affects the lateral sides of the nose and the nasolabial folds (skin folds that run from each side of the nose to corner of mouth), eyebrows, glabella (space between eyebrows and above the nose) and scalp. The chest, upper back and axillae (armpits) are less-commonly affected. It tends to be worse under moustaches and beards in men, so shaving is recommended. Cradle cap is a form of seborrhoeic dermatitis found in infants.
Diagnosis
Diagnosis is generally by physical examination. Depending on the part of the body affected, certain other conditions which display similar symptoms should be discounted. On the scalp it should be differentiated from psoriasis, atopic dermatitis, and impetigo. On the face, rosacea, contact dermatitis, psoriasis, and impetigo should be discounted and, on the trunk, pityriasis versicolor and pityriasis rosea must be discounted.
Treatment
Seborrhoeic dermatitis of the scalp (including dandruff)
Daily shampooing of the scalp with a medicated shampoo helps control scaling and pruritus. For best results, the shampoo should be left in place for five-to-10 minutes before rinsing.
Examples of classes of shampoos available include keratolytic shampoos, regulators of keratinisation, antimicrobial agents and antifungal agents.
Keratolytic agents soften, dissolve and release adherent scale seen in dandruff. The mechanism of keratolytic agents is not fully understood. Keratolytic agents include salicylic acid and sulphur. Preparations containing salicylic for the treatment of seborrhoeic dermatitis include Capasal shampoo and Cocois ointment. Cocois ointment also contains sulphur and coal tar. The fact that Cocois must be kept on the scalp for an hour before shampooing limits its use due to the fact this regimen is less convenient than other therapeutic shampoos available.
Regulators of keratinisation include zinc and tar. Zinc pyrithione (Head and Shoulders) is thought to control dandruff by normalising epithelial keratinisation, sebum production or both. Coal tar has been classically used to treat psoriasis; however, it is also effective in treating dandruff.
Problems of staining, its strong odour and messiness make tar products second-line for most patients. Tar products work by dispersing scales, which results in less malassezia colonisation. There were coal tar products on the market, including T-gel shampoo (Polytar liquid is no longer available in Ireland). Combination products of coal tar and other agents such as salicylic acid is common, ie, Capasal.
Antimicrobial agents such as selenium sulphide control dandruff via an anti-pityrosporum effect, rather than by an antiproliferative effect. Selsun is available over-the-counter in Ireland and is also used to treat pityriasis versicolor because of its effectiveness on the pityrosporum yeast.
Imidazole topical antifungals such as ketoconazole act by blocking the biosynthesis of ergosterol, the primary sterol derivative of the fungal cell membrane. Hydroxypyridones such as ciclopirox exert their antifungal effect by interfering with fungal cell membrane integrity and cell respiratory processes.
Shampoos containing the antifungal agents ketoconazole or ciclopirox are effective in the control of scalp seborrhoeic dermatitis. One study compared the use of ketoconazole 2% shampoo with selenium sulphide 2.5% shampoo in patients with seborrhoeic dermatitis.10 Both were significantly better than placebo and similarly effective in reducing irritation and itching; ketoconazole shampoo was better tolerated. Brands of ketoconazole shampoo available in Ireland include Nizoral. Another large, randomised trial found that ciclopirox shampoo was superior to placebo.11 Stieprox shampoo is the brand name for ciclospirox, available in Ireland.
Low-potency corticosteroids may be prescribed by doctors (POM) if other treatments prove ineffective. They should be used daily until improvement is seen. They should not be used for longer than a few days in seborrhoeic dermatitis. Alcohol-based solutions, gel, or foam preparations are most effective on the scalp. Locoid scalp application (medium potency), Elocon scalp application (potent) and Betnovate Scalp application (potent) are treatment options available in Ireland. Topical corticosteroids may hasten recurrences, may cause dependence because of a rebound effect, and are discouraged, except for short-term use.
Tea tree oil is a natural remedy derived from the leaves of an Australian tree called melaleuca alternifolia. It is often used for the treatment of dandruff. A trial that randomly assigned 126 people aged 14 or older with dandruff to four weeks of tea tree oil 5% shampoo or placebo found tea tree oil was significantly better.12 However, only one patient in each group achieved a complete response. There were no significant adverse events in this study; however, products containing tea tree oil have been associated with cutaneous allergic reactions,13,14 and tea tree oil may have estrogenic and antiandrogenic effects.15 The role of tea tree oil in the treatment of dandruff is uncertain.
Non-scalp seborrhoeic dermatitis
Antifungals, topical corticosteroids, or combinations of the two are the standard treatments for non-scalp seborrhoeic dermatitis. They are prescription-only medicines.
Topical and systemic antifungal agents are also effective. Ketoconazole shampoo is approved for this indication. Benefit has been shown with ketoconazole cream16,17 and oral terbinafine.18
As with seborrhoeic dermatitis of the scalp, low-potency corticosteroids should only be used short-term for non-scalp seborrhoeic dermatitis if other treatments fail. Creams or lotions are best tolerated on the face. Hydrocortisone 1% cream should be the first-choice corticosteroid in seborrhoeic dermatitis due to its mild potency.
Systemic fluconazole may help if seborrhoeic dermatitis is severe or unresponsive. The role of topical metronidazole agents in the therapy of seborrhoeic dermatitis has not been proven.
Conclusion
For mild-to-moderate seborrhoeic dermatitis, including dandruff, medicated shampoos containing salicylic acid or selenium sulphide are often effective treatment options. Combination treatments are useful in patients who do not respond to a single agent. Medicated shampoos containing ketoconazole, ciclopirox, selenium sulphide, coal tar, salicylic acid and zinc pyrithione should be used twice-weekly for at least a month and if necessary, indefinitely.
Ketoconazole 2% shampoo is the most effective treatment for moderate-to-severe seborrhoeic dermatitis. Combining ketoconazole with a steroid solution is effective where inflammation is a problem. Corticosteroids should never be used routinely. Ciclospirox shampoo is also very effective for moderate-to-severe seborrhoeic dermatitis.
References on request.